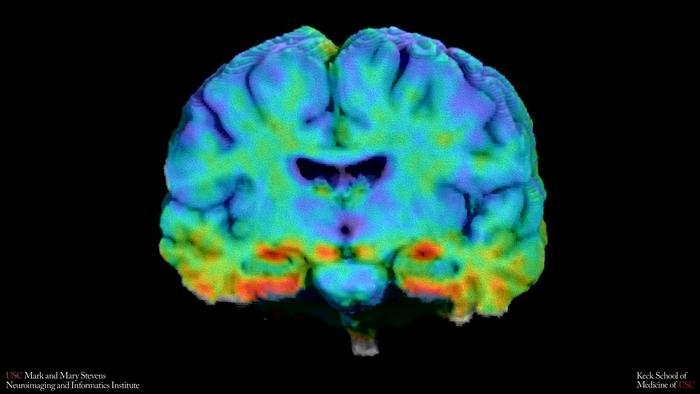
The scan takes about half an hour. You lie still while a radioactive tracer courses through your blood and binds to abnormal proteins in your brain, and the machine maps where those proteins have accumulated. It’s the most sensitive early-warning tool Alzheimer’s researchers have. And for decades, scientists have been calibrating what normal and abnormal look like based mostly on one group of people.
That assumption is now being tested in one of the largest and most diverse brain-imaging studies ever conducted in the US. The results suggest the standard biomarker picture of Alzheimer’s disease may not apply equally across racial and ethnic populations, and that some of the differences researchers are seeing could be partly an artefact of the imaging technology itself.
Researchers at the USC Mark and Mary Stevens Neuroimaging and Informatics Institute analysed tau PET brain scans from more than 1,500 older adults who were either cognitively normal or had mild cognitive impairment. Tau is a protein that forms tangles inside neurons, disrupting communication between brain cells; its accumulation in the medial temporal lobe, a region critical for memory, is considered one of the earliest warning signs of Alzheimer’s. Alongside tau, the team measured amyloid beta, the sticky plaques whose buildup typically precedes tau pathology in the standard model of disease progression.
What they found complicates that model considerably.
Black and Hispanic participants showed significantly higher tau levels in memory-related brain regions than non-Hispanic white participants, even when there was no evidence of amyloid plaques in those same brains. This was unexpected. The conventional sequence has amyloid accumulating first, then triggering tau spread; tau showing up before amyloid, and at higher levels, points to something else going on.
“Most Alzheimer’s research has been based on non-Hispanic white participants, and our results show that we can’t assume those patterns apply equally to everyone,” said Koral V. Wheeler, the study’s lead author and a PhD candidate at the Stevens INI. “If we want to advance precision medicine efforts for all communities, we need to understand how these brain markers behave across diverse populations.”
Part of the explanation, the team found, might not be biological at all. The tau PET tracer used in the study can produce spurious signals from structures near the hippocampus, particularly the choroid plexus, a small tissue that produces cerebrospinal fluid. When the researchers statistically controlled for this off-target binding, the apparent tau differences in Black participants shrank considerably, though didn’t vanish entirely in the cognitively normal group. Hispanic participants continued to show significantly elevated tau even after adjustment, suggesting something real is driving those levels up. A similar problem affected lateral temporal regions, where Hispanic participants initially showed higher tau; but after a separate correction procedure removed signal leaking in from the brain’s outer membranes, that difference disappeared entirely. The finding is a methodological warning: if these imaging tools aren’t properly validated in diverse populations, apparent biological differences may be partially artefactual.
Then there’s the cognition question, which turned out to be the most striking part of the study. For non-Hispanic white and Hispanic participants, having both high tau and amyloid plaques was associated with notably worse memory performance, the two pathologies compounding each other in a predictable way. But in Black participants, amyloid positivity didn’t strengthen the relationship between tau levels and memory decline in the same fashion. The proteins were there. The memory effects weren’t tracking them in quite the same way.
“This suggests that memory changes in Black adults may be influenced more strongly by factors beyond amyloid and tau alone,” said Meredith N. Braskie, the study’s senior author and an assistant professor of neurology at USC. “Vascular health, the presence of other health conditions, life-long stress exposure, and other social factors may play a prominent role and deserve closer study.”
That interpretation fits with broader patterns in the data. Black participants in the study had substantially higher rates of hypertension and type 2 diabetes compared to the non-Hispanic white group, conditions that promote vascular damage in the brain quite separately from Alzheimer’s pathology. Cerebrovascular disease can impair memory independently, and it may interact with tau and amyloid in ways the standard biomarker model wasn’t built to capture. Black adults are also disproportionately more likely to develop a mixed dementia, involving both Alzheimer’s and vascular pathology, which could help explain why the tau-amyloid-memory relationship looks different in this group.
The study’s participants came from the Health and Aging Brain Study-Health Disparities (HABS-HD), a multi-site effort that has assembled one of the most racially and ethnically diverse imaging cohorts in Alzheimer’s research. That diversity is what made the findings possible, and what makes them actionable. “Studies like this are essential for improving how we interpret the earliest biological signs of Alzheimer’s disease,” said Arthur W. Toga, director of the Stevens INI and co-lead of HABS-HD. “A more complete understanding of these imaging markers can help researchers better identify risk, track disease progression, and guide future prevention strategies.”
Future work will follow participants over time, allowing researchers to track how tau, amyloid, vascular health, genetics, and social factors interact as cognition changes. The study was cross-sectional, which means it captured a snapshot rather than a trajectory; longitudinal data will be needed to understand whether the different biomarker patterns seen across groups also predict different rates or routes of cognitive decline. What seems increasingly clear is that a biomarker playbook written from one population may leave clinicians with the wrong script when they encounter another.
Frequently Asked Questions
Why do Black and Hispanic adults show higher tau levels in Alzheimer’s brain scans? The reasons aren’t fully understood yet, but the USC-led study points to a combination of genuine biological differences and measurement artefacts. Some of the elevated tau signal in Black participants appears to come from off-target binding in a nearby brain structure called the choroid plexus, which can contaminate the scan rather than reflecting real tau pathology. Even after accounting for this, though, some differences remain, particularly in the hippocampus, and researchers suspect cumulative stress exposure, cardiovascular risk factors, and other social determinants of health may contribute to earlier or different patterns of tau accumulation.
What does it mean that amyloid didn’t predict memory decline the same way in Black participants? In the standard Alzheimer’s model, high tau combined with amyloid plaques is a powerful predictor of cognitive decline. In white and Hispanic participants in this study, that combination tracked closely with worse memory scores. In Black participants, the relationship was weaker and statistically non-significant. The researchers think this is because other factors, particularly vascular disease and conditions like hypertension and diabetes, may have a stronger influence on cognitive performance in this group, making amyloid and tau less reliable as standalone predictors of who will decline and when.
Could the imaging tools themselves be giving misleading results for some groups? Yes, and this is one of the study’s most important methodological contributions. The tau PET tracer used, called PI-2620, can produce false-positive signals in areas adjacent to the hippocampus and along the brain’s outer membranes. The USC team found that Black and Hispanic participants showed higher off-target binding in these regions than white participants, and that correcting for this binding changed the apparent size of the differences. The implication is that future studies need to validate and adjust PET imaging protocols when working with ethnically diverse participants, otherwise apparent biological differences may be partly an artefact of the scanner chemistry.
Is the APOE-e4 gene, the strongest known Alzheimer’s risk gene, equally relevant across racial groups? The study found that carrying the APOE-e4 allele was associated with higher tau levels overall, but this relationship didn’t differ significantly across racial or ethnic groups. The gene’s effect on how tau and amyloid interact, and on the tau-memory relationship, was similar across populations in this study. That said, earlier research has found that APOE-e4 has a weaker or more variable effect on Alzheimer’s risk in Black adults compared to white adults, and the authors note that genetic variation near the APOE region, which differs across ancestral backgrounds, may be a more nuanced predictor than the allele alone.
What happens next with this research? The HABS-HD study is ongoing and longitudinal, meaning participants will be rescanned over time. This will allow researchers to track whether the groups with higher tau levels in the absence of amyloid go on to develop cognitive impairment at different rates or via different pathways. Future analyses will also look more closely at cerebrovascular co-pathologies, social determinants of health, and how stress exposure across the life course shapes the brain’s biological ageing trajectory. The goal, ultimately, is a precision medicine approach to Alzheimer’s that actually accounts for the full diversity of who gets it.
There’s No Paywall Here, But We Depend On You!
If our reporting has informed or inspired you, please consider making a donation. Every contribution, no matter the size, empowers us to continue delivering accurate, engaging, and trustworthy science and medical news. Thank you for standing with us!
Related