Table of Contents
Melanoma is a malignant tumor that affects a group of cells called melanocytes. Also called pigment cells, melanocytes are cells specialized in the production of pigment in the skin, hair and eye. In most cases, melanoma begins on the surface of the skin, but it is possible that the tumor develops in the eyes or in internal organs, such as intestine and meninges.
Unlike many other cancers, the prognosis of melanoma is not alarming; the majority of patients who are diagnosed with early stage melanoma are completely cured. Although survival chances are high, melanoma can be life threatening. The disease can metastasize into lymph and/or other body parts, and decreases considerably the probability of recovery.
Melanoma Statistics

Melanoma is a very common cancer in Western countries; it represents about 10% of skin cancers and 1% of all cancers. Throughout the world, melanoma affects approximately 7 people per 100 000, killing about 48.000, according to the World Health Organization (WHO). It is estimated by the National Cancer Institute (NCI) that 39,080 men and 29,640 women (68,720 men and women) were diagnosed with melanoma of the skin in 2009; nearly 8,650 people died of the disease.
The incidence of melanoma varies with age. From 2002-2006, the median age at diagnosis for melanoma of the skin was 59 years of age. Ages and percentages of people diagnosed during that period (2002-2006) were approximately:
- 9% under age 20;
- 8% between 20 and 34;
- 4% between 35 and 44;
- 9% between 45 and 54;
- 8% between 55 and 64;
- 7% between 65 and 74;
- 8% between 75 and 84;
- 7% 85+ years of age.
Melanoma Causes
Melanoma is a very common skin cancer that concerns solely melanocytes, cells that lie in the skin’s epidermis, the middle layer of eye (iris, retina), in the inner ear (cochlea, stria), the digestive epithelium (tissue that lines the inside of the large and small intestine), and the meninges. Melanocytes play many roles in your body, among them pigmentation of skin and hair. Melanoma occurs when, due to certain pathogenic factors (see risk factors), some of these cells multiply uncontrollably to form a malignancy.
Intense or excessive sun exposure, especially during childhood, is the main factor responsible for the development of melanoma. This risk is even higher if you have fair skin. Although people with white skin are more often victims of melanoma, the cancer can also affect individuals with dark or pigmented skin. In black people, the cancer develops particularly on the palms (of hands) and soles (of the feet).
Depending on the characteristic of the cancer, melanoma is divided into many stereotypes; the most common include:
- Superficial spreading melanoma(SSM) – SSM represent about 70% of melanomas; it is the most common form of cutaneous melanoma in the lighter-skinned populations. Often developed on the sun-exposed skin areas, a mole of superficial spreading melanoma tends to grow horizontally for several months or years before taking its vertical extension where the lesion becomes thick and nodular.
- Nodular melanoma(NM) – the lesion of this form of melanoma tends to grow vertically. Due to its rapidity to grow, nodular melanoma is often considered as the most aggressive form of melanoma. It is characterized by a small blue-black or flesh colored spotting lump. Nodular melanoma lesions tend to penetrate deeper into the skin and bleed easily.
- Acral lentiginous melanoma –also known as subungual melanoma, acral lentiginous melanoma develops mostly on the palms, soles and under the nails. Unlike many forms of melanoma, acral lentiginous melanoma is more frequent among black and Asian people, and can develop on any area of the body which may or may not be exposed to sunlight. Acral melanoma is characterized by brown spot, flesh-colored nodules, which tends to resemble a wart or spotting tumor.
Melanoma Risk Factors
The most common risk factors of melanoma include:
- Sun-burn– sunburn is a major risk factor for melanoma. The risk is even higher if you have had sunburns during childhood. In addition, use of ultraviolet cabin can also increase the risk of having melanoma.
- Excessive sun exposure– studies have shown a connection between prolonged and repeated sun exposure and the occurrence of melanoma. The sun contains ultraviolet (UV) A and B, prolonged and repeated exposure to these rays tends to cause chemical changes in the DNA of the skin cells. Persistent changes can cause an uncontrolled proliferation of melanocytes (melanoma). This risk is even higher if you have fair skin or if the exposure is associated with repeated sunburns.
- Family history of melanoma– if you have family members suffering from melanoma, your risk increases. It is estimated that nearly 10% of melanomas are attributed to genetic predisposition.
- Fair skin– you are at higher risk of melanoma if you have fair skin, blond or red hair and light-colored eyes.
- Mole– having large moles (over 6 mm) in great quantity is at increased risk of developing melanoma.
- Genetic disorder– if you have xeroderma pigmentosum (XP), any less intense sun exposure can lead to skin malignancies: basal cell carcinoma, melanoma, etc.
- Exposure to carcinogens– your risk of having melanoma is higher if you are continuously exposed to these chemicals:
- coal tar
- creosote, a wood preservative
- Arsenic compounds in pesticides and radium.
- Weakened immune system– having a weakened immune system is an open door for all cancers including melanoma. The conditions that can weaken your immune system include:
- stress
- VIH / sida
- malnutrition
- chronic Leukemia
- cancer or/and treatment
- taking immunosuppressive drugs after an organ transplant.
Melanoma Symptoms
Melanoma is a cancer of the skin or mucous that can take different forms. The cancer can occur suddenly on a skin that was previously normal, or more rarely in a preexisting mole. Therefore, it is very important to consult a dermatologist as quickly as possible if you have a mole that undergoes a change in its:
- size
- shape
- color
- surface texture
- feeling (becomes painful or sensitive)
In addition, tell your dermatologist about any abnormal change in your skin. Like any cancer, melanoma must be detected and treated early for a better prognosis. Earlier the tumor is diagnosed, more chance you have to survive.
In early melanoma, you can observe a change in an existing mole or colored skin growth of a few millimeters. Unlike a regular skin lesion, a spot of melanoma is often asymmetrical and has an irregular border. After months or years, depending on the type of melanoma you have, the spot/mole evolves and undergoes changes in its size, shape, contour and color.
In addition, melanoma is often accompanied by the following dermal signs:
- changing the area surrounding the lesion
- presence of a growth or nodule
- extension of the lesion (it grows deeper into the skin)
- Itching – often associated with bleeding.
Melanoma Complications
The prognosis of melanoma is not bad when it is diagnosed and treated early. In other words, you have high chance to completely heal if the disease is detected at its early stage.
Nevertheless, an advanced melanoma can cause complications even after treatment. Thus, after treatment, a very prolonged monitoring is necessary to detect recurrence and ensure there are no other suspicious lesions. In the absence of an effective treatment and regular surveillance, the tumor can spread and give rise to metastases in the following sites:
- lymph nodes
- lung
- skin
- brain
- spinal cord
- liver
With metastases, your chance of survival decreases dramatically. To prevent metastases or/and recurrence, it is important to follow your doctor’s appointments and take all precautionary measures indicated by your oncologist.
Melanoma Diagnosis
Melanoma diagnosis can be done by a physical examination. During the exam, your dermatologist will examine your skin looking for lesions that can indicate melanoma. Your dermatologist may suspect melanoma based on the appearance of the lesion. In some cases, he can complete the exam by a dermatoscopic analysis, analysis of the skin lesion with a specific microscope.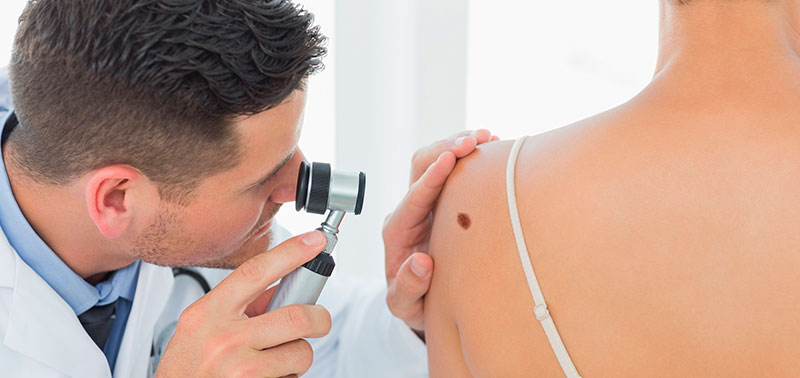
However, to confirm the diagnosis, a biopsy is necessary. Your physician will remove samples from the suspect lesion (biopsy) for laboratory analysis. This histological examination is essential to accurately confirm that you have melanoma. Besides the confirmation of the disease, biopsy can also you’re your doctor measure the exact deepness or thickness of the lesion in your skin.
Melanoma Stages
Once the cancer is found in your skin, it is necessary to determine its stage. In general, the stage of melanoma is determined according to its size and its extension – the spread of cancerous cells into lymph nodes or other parts of the body: lungs, brain, liver, bone, and spinal cord.
- Melanomain Situ –also called stage 0, melanoma in situ is the genesis of the cancer cells; your five-year survival chance is about 99.9%.
- Stage I –at this stage, the melanoma is invasive; although it is well localized, the cancer can spread to other areas of your body. Your five-year survival chance is less than 95%.
- Stage II –stage 2 is considered as a high risk melanoma; the cancer can spread into other areas of your body, and your 5-year survival rate is about 40-85%.
- Stage III –at stage 3, the cancer is more aggressive; the risk of regional metastasis increases. Your chance to survive 5 years after the diagnosis is estimated at 25-60%.
- Stage IV A –your survival chance has decreased considerably to 9-15%; the cancer is often associated with distant metastasis such as distant skin metastasis and lung metastasis
- Stage IV B– at this stage, the tumor has become more aggressive; the cancer has spread beyond your skin to other organs, such as lungs, liver and bone. Your five-year survival chance has decreased considerably.
Melanoma Treatment
Treatment of melanoma depends on many factors. Your doctor will base on the sage of the tumor, your age and health in general. Your recovery chances are higher when melanoma is diagnosed early. In general, melanoma treatment includes surgery, radiotherapy, chemotherapy and immunotherapy.
Surgical treatment
Surgical treatment is the essential treatment for an early stage melanoma. In fact, if the tumor is detected and removed early enough, no further treatment is necessary after the surgery. It is estimated that 80% of melanomas detected early are completely cured by surgery.
If the melanoma has spread into surrounding lymph nodes, your surgeon will perform a lymph node dissection to remove not only the tumor but also all the lymph nodes in the region near the tumor. In cases of metastatic melanoma, especially in the brain, your surgeon will perform surgery to relieve symptoms and improve the quality of your life. In this case, the surgery is considered as palliative treatment.
Chemotherapy
Chemotherapy is an important tool in the treatment of advanced or metastatic melanoma. It consists of using strong chemical agents to destroy the cancer cells by preventing them reproducing. Your doctor will consider the stage of the melanoma and your health to recommend you a protocol capable of eradicating the tumor. In general, elderly receive lower doses of chemotherapy. In addition, these chemotherapeutic agents can be administered alone or in combination. When many drugs are used, the treatment becomes more aggressive and can cause many side effects.
To increase your survival chance, chemotherapy can be used in combination with radiation therapy.
Radiotherapy (Radiation Therapy)
Radiotherapy is a loco-regional cancer treatment, consisting of exposing the tumor to ionizing radiation to shrink or eliminate it. Unlike chemotherapy, radiation therapy attacks cancer cells in a specific area. Radiation is often performed to treat advanced or metastatic melanoma to relieve symptoms or to shrink the tumor to make operable. As for the chemotherapy, radiation therapy can cause short or long term effects. Effects vary depending on the part of your body that has been irradiated.
Immunotherapy (Biological Therapy)
Also called biological therapy, immunotherapy is the use of substances (drugs) capable to strengthen the immune system to help your body fight the cancer. These drugs work by activating immune cells so they attack cancer cells and destroy them. Interferon and interleukin-2 are the two most used drugs in the treatment of melanoma; some of their adverse effects include:
- chills
- fever
- fatigue
- headache
- Muscle ache.
Melanoma Prognosis
After the treatment, there are chances of relapse. A second tumor may develop in other parts of your skin or even in distant tissues. Your survival rate depends largely on the stage of the tumor at diagnosis. However, the prognosis of melanoma is often excellent, unlike many other cancers.
Survival rate of melanoma differs from one race to another. According to the National Cancer Institute (NCI), the overall 5-year relative survival rate for 1999-2005 was 91.4%. Five-year relative survival rates by race and sex were approximately:
- 0% for white men;
- 9% for white women;
- 3% for black men;
- 4% for black women.
Melanoma Prevention
It is not always possible to prevent the occurrence of melanoma; you can however take steps to decrease your risk:
- Avoid tanning beds –tanning beds degage UVA rays that can penetrates into your skin and causes precancerous skin lesions; avoid them as long as you can.
- Regular medical visit– if you have been treated with melanoma, it is recommended that you have regular test every six months for two years and then annually. These preventive measures are needed to detect an early recurrence of a second melanoma.
- Check your skin regularly– check your skin regular to detect abnormal changes or changes in your moles. This is even more important if you were diagnosed with melanoma in the past.
- Avoid sun exposure– exposure to sunlight and ultraviolet radiation is the main risk factor for melanoma and therefore avoid them should be your first priority in preventing melanoma. In general, it is necessary to:
- avoid sunbathing
- wear protective clothes and hat when you walk under the sun
- avoid prolonged sun exposure between 10 am and 4 pm
- apply a protective sunscreen (20 index at least), renew every two hours and after swimming