Table of Contents
Sleep apnea is a respiratory disorder which occurs during sleep causing a decrease or cessation of breathing during. The disease is characterized by a momentary pause in breathing that can last more than 10 seconds and repeat multiple times during the night. Sleep apnea is often associated with snoring at night and tiredness during the day.
Scientists believe that sleep apnea occurs due to a narrowing of the pharynx associated with a relaxation of the throat muscle, leading to airflow obstruction and snoring.
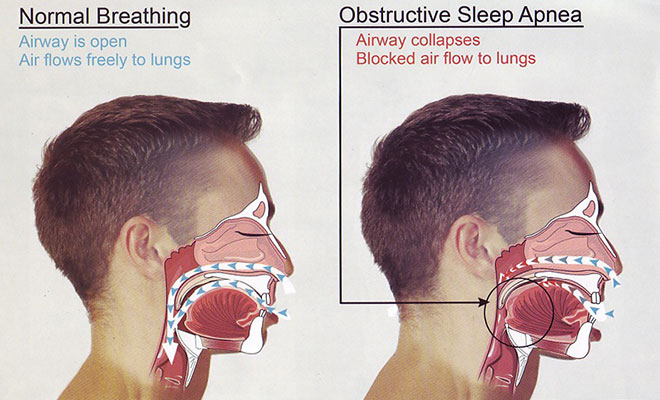 Most of the times, the disorder occurs when there is a closure of the airways, resulting in a temporary cessation of breathing; this form of apnea is called obstructive sleep apnea. Similarly, sometimes, there is no obstruction as a cause of apnea, the disorder is associated with a dysfunction of the centers of the central nervous system controlling the breathing; this condition is known as central sleep apnea. The Central sleep apnea is often associated with obstructive sleep apnea to form mixed sleep apnea or complex sleep apnea.
Most of the times, the disorder occurs when there is a closure of the airways, resulting in a temporary cessation of breathing; this form of apnea is called obstructive sleep apnea. Similarly, sometimes, there is no obstruction as a cause of apnea, the disorder is associated with a dysfunction of the centers of the central nervous system controlling the breathing; this condition is known as central sleep apnea. The Central sleep apnea is often associated with obstructive sleep apnea to form mixed sleep apnea or complex sleep apnea.
In addition to snoring and daytime fatigue, sleep apnea can have serious consequences on your health. At each pause or stop, your heart and brain know effects which can lead in the future to heart attack (myocardial infarction) or stroke.
Sleep apnea can occur at any age; before 60, however, it mainly affects men, although its incidence among women is increases with menopause. Certain diseases also increase the risk of sleep apnea. For example, frequency of sleep apnea is more than 35% higher among obese and hypertensive heart disease individuals.
Sleep Apnea Causes
Although as you get older your risk of the disease is increasing, sleep apnea can occur at any age, among both men and women. Several factors are suspected as triggers in the occurrence of sleep apnea symptoms: obesity, hormonal change, age, and physiological problems.
Obstructive sleep apnea – obstructive sleep apnea is the most common form of sleep apnea, representing about 9 out of 10 cases. However, it is less dangerous than central sleep apnea. You have obstructive sleep apnea when, during your sleep, you temporarily stop breathing because of an obstruction of the respiratory tract that blocks the normal passage of airflow. This obstruction can be caused by a relaxing of the muscles of the throat, an airway narrowing, tongue disorder or excessive fatty tissue in the throat.
In children, the disease is often linked to tonsils, swollen or enlarged adenoids. Swollen adenoids or tonsils in childhood may cause an abnormal craniofacial development and an upper airway obstruction, which can lead to obstructive sleep apnea.
Central sleep apnea – The Central sleep apnea is a rare form of sleep apnea; it is, however, more life threatening. Its causative factors are different from obstructive sleep apnea; medical researchers believe that the disease is resulted from failure of the brainstem or malfunction of the brain tissue that regulates breathing.
Central sleep apnea occurs mostly in people who have a problem in the brainstem such as infection, inflammation or tumor. The disease can be the result of persistent heavy alcohol consumption or prolonged drug abuse. Central sleep apnea may also be caused by heart disease or a chronic respiratory problem due to a cerebrovascular disease.
Sleep Apnea Risk Factors
Age – with age, the risk of sleep apnea increases.
Sex – sleep apnea is more frequent among men than it is in women.
Family history – if you have one or both parents with sleep apnea, your risk is higher.
Obesity – obesity and overweight can lead to accumulation of fat around the airway and related soft tissue. In some people, this excess of fat leads to obstructive sleep apnea.
Hormonal factors – studies have shown that sleep apnea is less prevalent among pre-menopausal women. In some women, hormonal change cause gaining of extra pounds in the upper body, which can cause obstructive sleep apnea.
Physiological problems – Anomalies in the jaw, tongue or soft palate can narrow the airway and cause obstructive sleep apnea.
Cigarette smoke – if you smoke, your chance of developing sleep apnea is higher.
Cerebral vascular accident (stroke) – about 50% of people with stroke also have a form of sleep apnea.
Sleep Apnea Symptoms
Symptoms of sleep apnea are often detected by the patient’s partner. In general, if you have either obstructive sleep apnea, central sleep apnea or mixed sleep apnea, you will experience at least one of the following symptoms:

- Snoring and breathing pause or cessation at night
- Nocturnal awakening associated with choking
- Dry mouth or sore throat in the morning
- Sweating during sleep
- Gastroesophageal reflux (GER)
- Frequent need to urinate at night (Nocturia)
- Lack of energy during the day
- Morning headaches
- Drowsiness during the day (hypersomnia)
- Concentration and memory problems
- Mood change, irritability or depression
Complications
If left untreated, sleep apnea may be responsible for insufficient oxygenation of the blood, which can lead to cardiac arrhythmia (also known as dysrhythmia), high blood pressure and even the occurrence of myocardial infarction (heart attack) or stroke.
Diagnosis
The diagnosis is based on an interview with your doctor, physical and clinical exams such as polysomnography and oximetry. Your doctor will do the physical exam and ask you a few questions in order to know if you have sleep apnea, and prescribe you more specific exams.
Oximetry – this is a noninvasive medical procedure used to measure or determine the amount of oxygen in your blood. During the procedure, the specialist will use a medical device called oximeter to examine the color of your blood. The oximeter consists of a sensor made of a red light source and a light sensor connected to an analyzer. You will be asked to place a finger between the source of the red light and the sensor that analyzes the amount of light transmitted.
In general, an oxygen-rich blood is redder than blood low in this molecule; this difference is quantified to determine the oxygen saturation. This saturation is expressed in percentage; it is between 95 and 100% in normal subjects but lower in smokers and those suffering from sleep apnea. If the exam reveals any suspicious about the disease, your doctor will recommend a polysomnography to confirm the diagnosis.
Polysomnography – polysomnography is a complex examination which is performed in a sleep disorder center or at home. It consists of registering and analyzing your blood oxygen levels and different parameters of sleep: breathing, snoring, your heart and lung functions, brain activity, and your arm and leg movements.
Sleep Apnea Treatment
Before starting any medical or/and surgical treatment, it is important to reduce or eliminate factors that may cause or worsen the symptoms of the disease:

Lose weight – if you are diagnosed with sleep apnea, it is crucial to lose weight from the diagnosis. Because there is a close relationship between overweight and severity of sleep apnea symptoms, nearly one in two obese has a sleep disorder.
Change position to sleep – most of the times, soft tissues are located on the front of the larynx, in some individuals, sleep on the side can help reduce the frequency of sleep apnea and improved their sleep. Therefore, if you have the disease, try this simple technique.
Avoid substances that aggravate snoring – some substances have a negative effect on your respiratory tract; they tend to aggravate snoring and sleep apnea symptoms. Therefore, if you are diagnosed with sleep apnea, you should:
- Stop smoking
- Stop drinking alcohol
- Stop taking sedatives or tranquilizers
Medical treatment
Continuous positive airway pressure (CPAP) – CPAP is the use of an assisted breathing device to treat certain respiratory and sleep disorders, particularly obstructive sleep apnea. This therapy is performed primarily in patients with repeated and prolonged breathing cessation (10 seconds to 2 minutes) during sleep. During the night, you will be recommended to wear a mask over your nose and mouth. The device is connected to a compressor that blows air at a prescribed pressure; this creates a cushion of air at the back of the throat and prevents it from closing.
This treatment can be 100% effective in certain patients; some people, however, feel the machine uncomfortable. If you cannot stand the CPAP, your doctor will prescribe you an adjustable airway pressure device.
Adjustable airway pressure devices are sometimes employed as an alternative to nasal continuous positive airway pressure (CPAP) therapy in minor sleep apnea. It allows movements of the lower jaw in three dimensions, therefore, reduce snoring, pauses and/or breathing cessation at night.
Wearing oral appliance – wearing oral appliance is, sometimes, alternating with continuous positive pressure. It allows you to reposition the lower jaw and tongue so that air flows more easily; therefor, reduces snoring and obstructive sleep apnea.
Surgical treatment
Surgery is used in some severe cases of apnea to restore a normal circulation in the upper airways. The most used surgical methods include: uvulopalatopharyngoplasty (UPPP), bimaxillary advancement (Bi-Max), and tracheostomy.
Uvulopalatopharyngoplasty – this surgical procedure consist of removing tissue in at least one of the following organs:
- Uvula
- Soft palate
- Tonsils
- Adenoids
- Pharynx.
This procedure is performed under general anesthetic, and it is not always successful.
Bimaxillary Advancement (Bi-Max) – also called maxillomandibular advancement, Bi-Max is a surgical procedure consisting of moving the top jaw (maxilla) and the bottom (mandible) forward to relieve sleep related breathing disorder. Depending on the anomaly causing the disorder, your surgeon may perform genioglossus advancement (pulling forward the base of the tongue) along with the bimaxillary advancement for better result.
Tracheostomy – the tracheostomy is rarely practiced in the treatment of sleep apnea; it is reserved for severe cases of apnea or when there is a life threatening condition such as cancer of the larynx. It consists of a surgical opening in the trachea below the larynx to ensure a permanent permeability of airways.



