Table of Contents
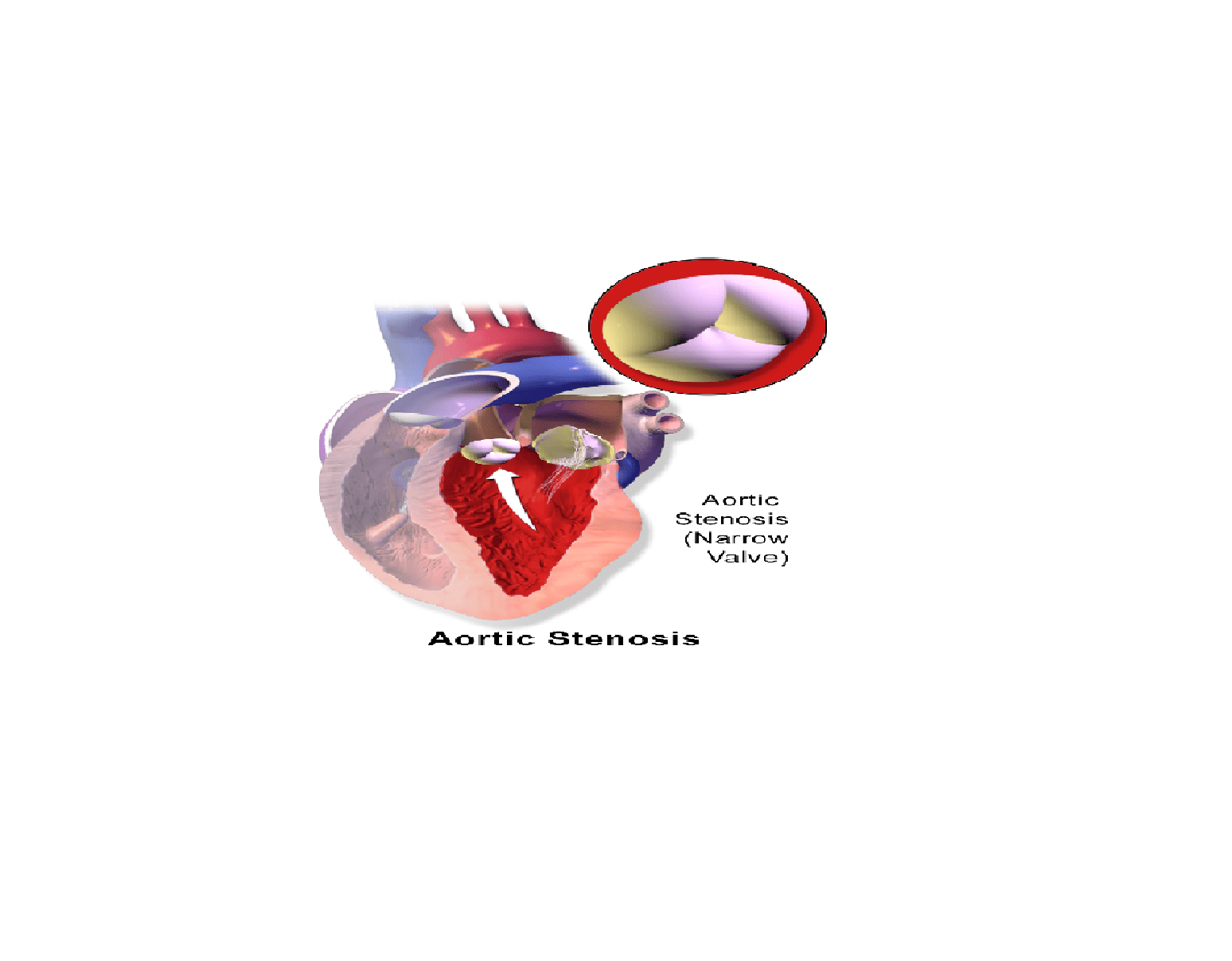
Aortic Stenosis
Normally, the inner surface of the aortic cavity in adults is 2.5 to 3.5cm2. Aortic stenosis, also known as aortic valve stenosis, (AS or AoS)) occurs when the aortic valve area becomes narrowed to less than 2.5 cm2, causing obstruction of blood flow from the heart into the aorta and the rest of the body. If the cavity is so narrowed that becomes less than 1cm2, the obstruction is severe and requires immediate surgical intervention, valve replacement surgery. Absence of treatment can lead to heart failure or even sudden death.
In other words, aortic stenosis is a cardiac disease characterized by a narrowing of the aortic valve. Aortic stenosis is the most common disease of the heart valves; it is responsible for approximately 25% of heart valve diseases in adults. The risk of the disease increases with age. According to Edward Morgan, the percentage of people suffering from aortic stenosis is estimated at:
- 2% in people over the age of 65
- 3% in people over age 75
- 4% in people over age 85.
Aortic Stenosis Symptoms
In most cases, aortic stenosis produces no symptoms at the beginning; the disease is often discovered during an examination for another medical condition. If the obstruction is severe, or if the narrowing evolving for many years, symptoms may emerge:
- Dizziness
- Shortness of breath
- Heart palpitations
- Loss of consciousness (syncope)
- Heat murmur of low intensity
- Chest pain suggestive of angina pectoris
- Tiredness and fatigue occurs during exercise or permanently
- Left-sided heart failure symptoms: cough, confusion, slowing of physical activity (psychomotor retardation), abdominal pain, nausea, etc…
Complications
Although a life threatening disease, aortic valve stenosis can be treated or cured definitely by surgical treatment; if left untreated however, an aortic stenosis can cause serious complications:
- difficulty breathing
- endocarditis
- heart failure
- irregular heart rhythms
- Pulmonary edema.
Aortic Stenosis Causes
The heart is composed of four chambers, two atria (upper chambers) and two ventricles (bottom chambers). Prevention of backflow from the ventricles into the atria during systole is assured by four small valves: tricuspid valve (also known as right atrioventricular valve), pulmonary valve (also called pulmonic valve), mitral valve (sometimes called bicuspid valve or left atrioventricular valve) and aortic valve. The aortic valve is located between the left ventricle and the aorta, the largest artery in the body. Aortic stenosis occurs when there is a reduction or narrowing of the surface of the aortic valve, preventing blood from flowing from the heart to other parts of the body.
Risk factors
Several factors can lead to development of aortic stenosis; the most common include:
Medications – cancer treatment (radiation therapy) or prolonged use of ergotamine (a drug used in the treatment of migraine headaches) can damage your aortic valve, causing aortic stenosis.
Metabolic disorders – some metabolic disorders such as high blood cholesterol (hypercholesterolemia) may play a role in the occurrence of aortic stenosis.
Rheumatic fever – aortic stenosis can be the result of an untreated or chronic rheumatic fever due to complications of a streptococcal infection. In this case, there is a thickening of the valve.
Congenital heart defect – in more than half of aortic stenosis patients, the disease is the result of a birth defect of the valve. These patients, instead of having three cusps (tricuspid valve), they have two cusps (bicuspid valve). A bicuspid aortic valve (BAV) is a major cause of aortic stenosis.
Aortic valve calcification – a progressive calcification of the aortic valve is sometimes responsible for the development of aortic stenosis. Aortic valve calcification is often due to age, usually occur after 60.
Diagnosis
The first step in aortic stenosis diagnosis is a physical exam. During the examination, your doctor will look for signs characteristic of the disease: heart murmur, heart palpitations, etc. In addition, your cardiologist will ask you questions about your medical history in order to discover disease related to aortic valve stenosis. However, to confirm the diagnosis other tests must be done.
Chest x-ray – this radiographic procedure is performed to produce images of the heart muscle, lungs and bones forming the thoracic cage. It allows your doctor to detect abnormal shape and size of the heart. In addition, it allows your physician to confirm the presence of a valve disorder and provides important details about your heart condition and its severity.
Echocardiogram – during an echocardiogram, the technician uses ultrasound to create picture of your heart. The waves recorded help him determine the shape, texture and movement of the valves and the volume and function of the cardiac chambers. In addition, this imaging technique is performed to determine the risk of clots inside the heart muscle.
Generally, an echocardiogram is recommended if during the physical examination, your doctor suspects that your heart produces abnormal sounds, or if you experience breathlessness, palpitations or chest pain.
Electrocardiogram (ECG) – This test is done to study the functioning of your heart by measuring its electrical activity. Each heartbeat produces an electrical impulse in your heart that contracts the heart muscle so it pumps blood to the body. By measuring the time the electrical impulse takes to travel through the heart, your cardiologist can determine if electrical activity is normal, fast or irregular.
In addition, an electrocardiogram allows your cardiologist to determine if your heart is dilated or overworking. Your cardiologist will recommend an ECG if physical examination shows signs of arrhythmia, palpitations, dizziness, fatigue or chest pain.
Cardiac catheterization – your doctor may recommend a cardiac catheterization if you have signs of heart valves malfunctioning or heart failure. It consists of introducing a thin catheter through your blood vessel in your arm or groin into your heart chambers to measure pressure and blood oxygen saturation level. In addition, this examination allows your doctor to detect reflux of blood from the aorta to the left ventricle.
Aortic Stenosis Treatment
Your cardiologist may treat you with drugs or surgery, depending on the severity of the disease. Medications, however, are used as symptomatic treatment; they aim at relieving the symptoms of the disease, not the aortic valve stenosis itself.
Drug Treatment
Vasodilators – this class of drugs are often recommended to treat aortic valve stenosis. They are substances that help dilate blood vessels by relaxing the smooth muscles of their walls. Vasodilators are recommended to be used in small doses to avoid excessive reduction of ventricular filling, which can lead to sudden and dangerous fall in blood pressure.
Diuretics – diuretics are used in the treatment of hypertension, heart failure, some edemas, portal hypertension (high blood pressure in the large vein that brings blood from the intestine to the liver) and hypokalemia (low potassium level in the blood). They work by increasing the secretion of urine. Your doctor can prescribe them in cases of heart failure to improve breathlessness. However, diuretics do not reduce the progression of the disease.
Satins- also called HMG-CoA reductase, satins are a class of cholesterol lowering medications that your doctor can recommend you to take to slow the progression of an aortic valve stenosis. Their results are, at present, mixed; therefore, to increase your chance of getting good results from them, live a healthy lifestyle, adopt a heart healthy diet, and do not smoke.
Antibiotics – As with valvular heart disease, there is a risk of infective endocarditis associated with aortic valve stenosis. Your doctor may recommend that you take appropriate antibiotics to prevent this complication.
Surgical treatment
If surgery is necessary, mostly, your surgeon will do either an aortic valve replacement or a balloon valvuloplasty.
Aortic valve replacement – the surgical replacement of the valve is the ideal treatment when the aortic stenosis is accompanied with symptoms: shortness of breath on exertion, angina, discomfort on exertion, etc. The surgeon can also proceed to surgery in asymptomatic aortic valve stenosis if successive and frequent examinations show that the valve is gradually shrinking.
During the procedure, a cardiopulmonary bypass machine can be established to irrigate the heart and lungs in blood and oxygen during the surgery (open heart surgery). The goal of the intervention is to remove the diseased valve and replace it with an artificial valve; the prosthesis can be mechanical (metal or synthetic materials) or biological if it consists of a human tissue or animal.
The mechanical valve is solid; it requires an anticoagulant treatment for life to prevent blood clots from forming on or near the valve.
The biological valve does not need an anti-coagulant, but it may only last up to 10 years, requiring a new valve replacement.
Non surgical techniques
Balloon valvuloplasty – unlike aortic valve replacement, balloon valvuloplasty does not require an open heart surgery. Your surgeon places a balloon catheter inside the narrowed heart valve to stretch it open. The balloon valvuloplasty is not new; it has been developed since the late 1980s, but rarely used due to complications and constant repetition. Even when performed, balloon valvotomy is not to be recommended, except for some adolescent congenital defects, according to the ACC / AHA 2006 Guidelines for the Management of Patients with Valvular Heart Disease.
Bioprosthetic aortic valve replacement – this new method occurred around the year 2002. During the procedure, the implant is made by catheterization without the need for heart surgery. It is being evaluated in the treatment of aortic valve stenosis; the future will show what it will bring.
Aortic Stenosis Prevention
The two best ways to prevent aortic valve stenosis is by keeping your blood pressure under control and preventing rheumatic fever. Having healthy blood pressure levels requires regular exercise, consumption of health diet, avoidance of bad stress and cigarette smoke, including second hand smoke.
If you have strep throat, see your health care provider and follow the treatment as prescribed. Rheumatic fever is often the consequence of untreated or poorly treated strep throat. Prevention of recurrences is based on oral or intramuscular injection of antibiotics for at least 5 months. Talk to your physician for more information on aortic valve stenosis prevention.
References :
1 – Pellikka PA, Sarano ME, Nishimura RA et als. Outcome of 622 adults with asymptomatic, hemodynamically significant aortic stenosis during prolonged follow-up
2 – Rosuvastatin affecting aortic valve endothelium to slow the progression of aortic stenosis [archive], Luis M. Moura, Sandra F. Ramos, José L. Zamorano, Isabel M. Barros, MDLuis F. Azevedo, Francisco Rocha-Gonçalves, Nalini M. Rajamannan, J Am Coll Cardiol, 2007; 49:554-561
3 – A Randomized trial of intensive lipid-lowering therapy in calcific aortic stenosis”” [archive], S. Joanna Cowell, David E. Newby, Robin J. Prescott, Peter Bloomfield, John Reid, David B. Northridge, Nicholas A. Boon, New Eng J Med, 2005;352:2389-2397
4 – Roques F, Michel P, Goldstone AR et als. The logistic EuroSCORE [archive], Eur Heart J, 2003;24:881–882
5 – Edwards FH, Grover FL, Shroyer AL et als. The Society of Thoracic Surgeons National Cardiac Surgery Database: current risk assessment [archive], Ann Thorac Surg, 1997;63:903–908
6 – ACC/AHA 2006 Guidelines for the Management of Patients with Valvular Heart Disease“. American Heart Association.
7 – Clinical anesthesiology By G. Edward Morgan, Maged S. Mikhail, Michael J. Murray
8 – Miller JD (June 2013). “Cardiovascular calcification: Orbicular origins”. Nature Materials 12 (6): 476–8. doi:10.1038/nmat3663. PMID 23695741.
9 – Figuinha, FC; Spina, GS; Tarasoutchi, F (March 2011). “Heyde’s syndrome: case report and literature review”. Arquivos Brasileiros de Cardiologia 96 (3): e42–e45. doi:10.1590/S0066-782X2011000300017. PMID 21484065.
10 – Ricardo Zalaquett, Cristóbal Camplá, et al. (2005). “Cirugía reparadora de la válvula aórtica bicúspide insuficiente”. Rev Méd Chile, 133(3): pp. 279-86. ISSN 0034-9887
11 – Hans-Joachim Schäfers: Current treatment of aortic regurgitation. UNI-MED Science, Bremen, London, Boston 2013, ISBN 978-3-8374-1406-6.
12 – Mayo Clinic > Aortic valve stenosis > Treatments and drugs Retrieved September 2010
13 – Christopher M. O’Connor (2005). Managing Acute Decompensated Heart Failure a Clinician’s Guide to Diagnosis and Treatment. London: Informa Healthcare. p. 406. ISBN 9780203421345