Table of Contents
Psoriasis is a chronic skin disease characterized by eruption of itchy, dry and red patches on your scalp, nails, knees, elbows, feet, hands, genitals, or your whole body. Psoriasis is an autoimmune disease; that is, your immune system turns against normal tissues in your body causing an excessive skin cells production.
Psoriasis is a common autoimmune disorder, affecting approximately 2 to 3% of the world population. Its cause is unknown, but there is probably a hereditary factor; your risk of developing psoriasis is 5 to 10% higher if you have a parent affected. In addition, race may play a role in its onset; psoriasis is more common among white skin individuals.
Unlike many other incurable diseases, psoriasis is not contagious or life threatening; it may, however, make your life miserable when it develops on the palms of your hands, your soles (the bottom of your feet), in the folds of your joints, or on your genitals. The disagreeable effects of the lesions may impact negatively your emotional, social and personal life.
Psoriasis Symptoms
In general, psoriasis is characterized by scaly patches called psoriatic plaques. The plaques are often quite large, but also occasionally occur as small papules. Sometimes they have the size and shape of a coin. The disease can also develop on skin folds of your armpit or groin, or the palms of your hands or soles. However, these symptoms vary from one person and depending on the type of psoriasis:
:max_bytes(150000):strip_icc()/psoriasis-symptoms-5b6880af46e0fb002538c5ad.png) Plaque psoriasis – also called psoriasis vulgaris, plaque psoriasis accounts for nearly 80% of cases of the disease; which makes it the most common form of psoriasis. In psoriasis vulgaris, skin lesions are red, irritated, itchy and scaly. When the plaques are scraped off, the area gives an appearance of punctate bleeding spots, Auspitz’s sign. Symptoms of plaque psoriasis can develop anywhere in your body including the soft tissue inside your mouth and genital areas.
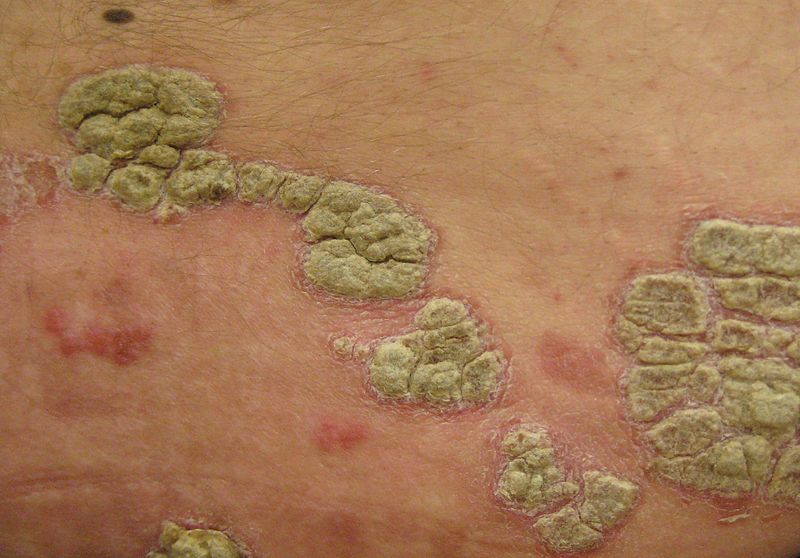
Plaque psoriasis – also called psoriasis vulgaris, plaque psoriasis accounts for nearly 80% of cases of the disease; which makes it the most common form of psoriasis. In psoriasis vulgaris, skin lesions are red, irritated, itchy and scaly. When the plaques are scraped off, the area gives an appearance of punctate bleeding spots, Auspitz’s sign. Symptoms of plaque psoriasis can develop anywhere in your body including the soft tissue inside your mouth and genital areas.
Guttata psoriasis – this skin condition is uncommon in comparison with psoriasis vulgaris. It occurs mostly following a bacterial infection. It is characterized by a scattering of small scaly crusted spots over large areas of your body mainly on your legs, lower abdomen, lower back, forearm, chest, or your scalp. Psoriasis guttata does not cause any plaques but small, red, water –drop- like spots which tend to disappear on their own without leaving any complications.
Erythrodermic psoriasis – erythrodermic psoriasis is a rare but severe form of psoriasis. It tends to cause inflammation of the skin and may affect your entire body. Most of the times, erythrodermic psoriasis is due to complication or extension of an existing psoriasis; rarely, development of a new erythrodermic psoriasis can occur. The affected area becomes red, sometimes wet, edematous and covered with fine scales. In addition, erythrodermic psoriasis can cause various thermal regulation problems such as chills, cardiovascular disorders, and sometimes fever.
Pustular Psoriasis – this is an uncommon form of psoriasis. It is usually localized on the palm of your hands, feet and fingertips. Its occurrence consists of multiple small pustules lesions – small, inflamed, pus-filled lesions. Usually, the patches are milky white or yellowish white, which can be generalized (generalized pustular psoriasis) or localized (localized pustular psoriasis). Pustules lesions have a tendency to coalescence, they come together so as to form one whole.
Inverse psoriasis – also called Inverted psoriasis, inverse psoriasis affects mostly the skin folds such as armpits, groin, under the breasts, under stomach (mostly in overweight people), the genital areas and rarely the belly button. It is characterized by bright red inflamed patches, which can be smooth and little scaly.
Nail psoriasis – nail psoriasis is another frequent form of psoriasis; it occurs in more than 50% of cases of psoriasis. Usually, it is characterized by an abnormal growth and discoloration of the fingernails and toenails. As the disease worsens, you will observe lines going across the nails, which make them (the infected nails) become loose and crumble. In addition, the skin under the infected nails becomes thick.
Psoriatic arthritis – this form of psoriasis affects your joint and connective tissue. It is characterized by a chronic inflammatory arthritis and skin lesions. The inflammation affects mostly the neck, back, fingers and the spine. Although rare, complications can lead to inflammatory eye disease, joint damage and permanent deformity. Psoriatic arthritis represents about 10 to 15% of all psoriasis incidences.
Psoriasis Causes
In most cases, precise causes of psoriasis are unknown; there are, however, factors that are sometimes suspected: familial, nutritional, autoimmune disorder, microbiological and environmental.
 Genetic predisposition – a great majority of psoriasis patients have one or more members of their family also suffering from the disease. In addition, it is shown that there is a higher risk among children born to parents who have psoriasis to develop the disease; nearly 30% of psoriasis patients have a family member struggling with the disorder.
Genetic predisposition – a great majority of psoriasis patients have one or more members of their family also suffering from the disease. In addition, it is shown that there is a higher risk among children born to parents who have psoriasis to develop the disease; nearly 30% of psoriasis patients have a family member struggling with the disorder.
Nutrition – Some researchers believe that a poor digestion or unhealthy diet can play a significant role in the development of psoriasis. Nutritional factors that can be linked to psoriasis include:
- Deficiencies in vitamin A and zinc
- Incomplete digestion of proteins, which lead to formation of toxins in the body
- Heavy consumption of alcohol, animal fat, dairy products and all products that can cause overload in the liver.
Immune disorder – It is also believed that dysfunction of the immune system may participate in the development of psoriasis. In people with the disease, the T lymphocyte or T cell (a white blood cell that detect and fight off pathogenic substances) mistakenly attack healthy skin cells, leading to formation of psoriatic plaques.
Medications – Some medications such as beta-blockers, lithium, iodides and antimalarial drugs seem to exacerbate psoriasis symptoms.
Some of factors that could trigger psoriasis symptoms include:
- Stress
- Smoking
- Cold weather
- An injury to the skin
- An immunological reaction against another disease, like chickenpox
- Systemic infection such as pharyngitis or strep throat
- Prolonged exposure to sunlight or chemicals such as disinfectants or paint thinners.
Psoriasis Diagnosis
In most cases, psoriasis is diagnosed solely on the basis of physical examination. Your doctor recognizes the disease by observing the nature and location of the symptoms. During the examination, the dermatologist may scrape the areas affected with the psoriasis with a wooden spatula to loosen and remove the scales.
However, if there are complications, your dermatologist can take a small sample of your skin to be examined under a microscope (biopsy) to rule out other skin conditions that have symptoms similar to psoriasis: seborrheic dermatitis, eczema, lupus, syphilis, skin cancer, etc.
Psoriasis Treatment
There is no curative treatment to completely eradicate psoriasis; despite the effectiveness of the medications, you can never be sure that the disease will not return. However, there are effective medical treatments that are able to control the symptoms, reduce or eliminate the lesions and improve your life. In addition, treatments vary depending on the type of psoriasis, location and its severity.

There are two types of treatment for psoriasis:
Topical treatment – creams and ointments are often effective in mild to moderate forms of psoriasis. They are used to relax the tissues, reduce inflammation, and soften the skin. Emollient bath or keratolytics can be used to facilitate exfoliation of excess epidermal cells. The reduction of redness can be done by a group of products called reducers: coal tar, anthralin, calcineurin inhibitors, topical corticosteroids, and Vitamin D analogues.
- Coal tar – Coal tar is a brown or black over-the-counter medication often used in the treatment of psoriasis. In fact it is considered as the most ancient form of psoriasis treatment. When used regularly, coal tar can reduce inflammation and scaling with no or few side effects. Some products containing coal tar include Balnetar, Psoriasin and Tegrin.
- Vitamin D analogues – Vitamin D and its analogues are sometimes effective in the treatment of psoriasis. They are used to reduce or control the excessive growth of skin cells. The most common drug used in the US is Calcipotriene (Dovonex or Daivonex). Calcipotriene is available in the form of cream, ointment and scalp solution. Calcipotriene can be sued alone or in combination with other topical medications. Usually, improvement is seen within 2 weeks of regular use.
- Corticosteroids – corticosteroids are used to reduce inflammation and stop outbreaks in mild to moderate psoriasis. To start the treatment, your dermatologist will likely prescribe to you low-potency corticosteroid ointments. They reduce inflammation and itching by suppressing your immune system. In some patients, however, low-potency corticosteroids cause a form of insensitivity, which requires increasing doses over time. In general, corticosteroids are used for a short period of time and on limited areas of the body. The problem is that in the majority of people, the plaques tend to come from the discontinuation of the treatment.
- Anthralin – this drug is applied on the skin to dry psoriatic plaques and remove the scales. It controls the abnormal growth of skin cells, thus preventing future outbreaks. For most people, anthralin stop the symptoms of psoriasis and prevent their recurrence for a long period of time. However, anthralin usually starts working after several weeks of application. In addition, it tends to stain your skin, clothing and bedding.
- Calcineurin inhibitors – calcineurin inhibitors (tacrolimus and pimecrolimus) are mainly used to treat atopic dermatitis symptoms. Studies have shown, however, that the drug can also provide relief in the life of people struggling with moderate psoriasis.
Prolonged use of calcineurin inhibitors can lead to serious health problems including lymphoma and skin cancer.
- Topical retinoids – Retinoids are commonly used in the treatment of acne. However, tazarotene (Tazorac, Avage), a derivative of vitamin A, works effectively in fighting psoriasis symptoms. Retinoids are used mainly in the treatment of pustular psoriasis. It is available in ointment.
Before using tazarotene, it is important to talk to your doctor if you are pregnant or may become pregnant; although rare, the drug can cause birth defect. In addition, application of tazarotene should always be associated with sunscreen to prevent sun damage to your skin.
Phototherapy – if other treatments do not produce any satisfying results, your dermatologist will expose your skin to ultraviolet (UV) radiation to treat the psoriasis; this form of psoriasis therapy is called phototherapy; depending on method used, phototherapy may include:
- Sunlight – daily sun exposure in moderation can have a curative effect on mild to moderate form of psoriasis. However, direct and prolonged exposure to sun rays can be harmful. You must follow this treatment after the advice of a medical specialist. In addition, you must monitor closely how your body reacts to sun exposure.
- UVB phototherapy (ultraviolet therapy) – this is a form of psoriasis treatment using artificial ultraviolet light. UVB phototherapy is realized with tubes providing specific wavelength specific (311-313nm). The therapy is usually performed three times a week for a few minutes per session.
UVB phototherapy can be effective in combating the symptoms of psoriasis. However, it must be done under strict medical supervision to avoid health problems such as skin cancer. In addition, it is necessary to use a natural moisturizer during the therapy to prevent skin problems including but not limited to redness, itching and dryness.
- Photochemotherapy or PUVA therapy – this method consists of exposing the infected area of your skin to ultra-violet A, after taking a light-sensitizing medication called psoralen (or psoralene). Exposure to ultraviolet A alone does not always give good results. Therefore, 1½ to 2 hours before the therapy, you will be recommended to take psoralen tablets to allow skin sensitization. Typically, 3 sessions per week for about 5-15 minutes are sufficient.
However, PUVA therapy is less used due to its multiple side effects: nausea, headache, burning and itching, and wrinkled skin. In addition, the therapy may increase your risk of getting melanoma, a serious form of skin cancer. Talk to your doctor and think twice before doing this therapy.
Systematic Treatment – For the most severe forms of psoriasis, your doctor can prescribe systemic treatments in which the medications are spread throughout your body. These drugs can be taken orally or by injection:
Methotrexate – is an antagonist of folic acid. It used in the treatment of a variety of diseases associated with abnormally rapid cell growth including psoriasis. Methotrexate is primarily used in psoriatic arthritis to suppress inflammation. Side effects may include:
- Weakened immune system
- Mouth sores
- Stomach upset
- Hair loss
- Headache and dizziness
- Skin rash and itching
- Although rare, methotrexate can cause toxicity of the liver, kidneys and lungs
Retinoids – retinoids are vitamin A derivatives; they are recommended in moderate to severe psoriasis, or when the other alternatives fail to produce a satisfying result. Those drugs are, however, teratogenic; they can impact the growth and development of embryo or fetus not only during the treatment but also two years after the last dose. Women of reproductive age should not take retinoids if you consider becoming pregnant.
- Cyclosporin: this drug is an immunosuppressant commonly is used in psoriasis. The drug can be effective, but always accompanied by side effects due to the immune system weakness effect. If you are taking cyclosporine, it is important to avoid all pathogenic factors because your risk of infection and other serious health problems is higher.
- Other medications that your dermatologist may prescribe you include: Hydroxyurea, alefacept (Amevive), etanercept (Enbrel) and infliximab (Remicade).
It is important during the treatment to avoid alcohol and tobacco; adopt a healthy diet containing omega-3 fatty acids. In addition, regular exercise and good night sleep (at least eight hours) are vital.
References:
Andressen C, Henseler T, Inheritance of psoriasis. Analysis of 2035 family histories, Hautarzt, 1982;33:214–217
TheFreeDictionary: The American Heritage® Dictionary of the English Language, Fourth Edition copyright ©2000 by Houghton Mifflin Company; coalescence