Table of Contents
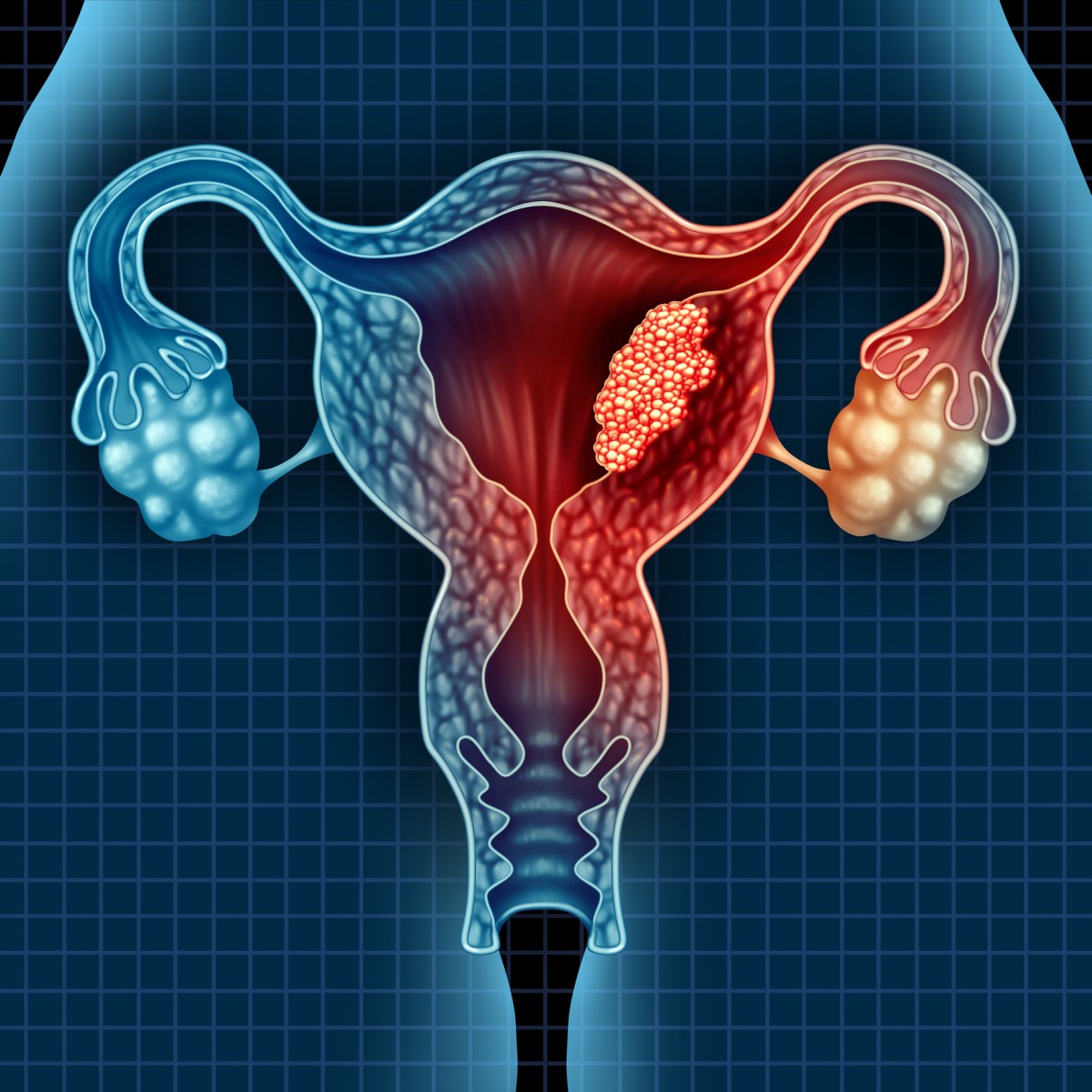
Also called endometrial cancer, uterine cancer is a cancer that forms in the cells that line the inside of the uterus. Generally, Uterine cancer develops after menopause; its evolution is slow, which makes it has a good prognosis. The main treatment is removal of the uterus and ovaries. In some cases, radiotherapy and chemotherapy may be associated with the surgery to increase chance of recovery. In fact, five-year survival rate for all stages of uterine cancer can be 90-95% when diagnosed and treated early.
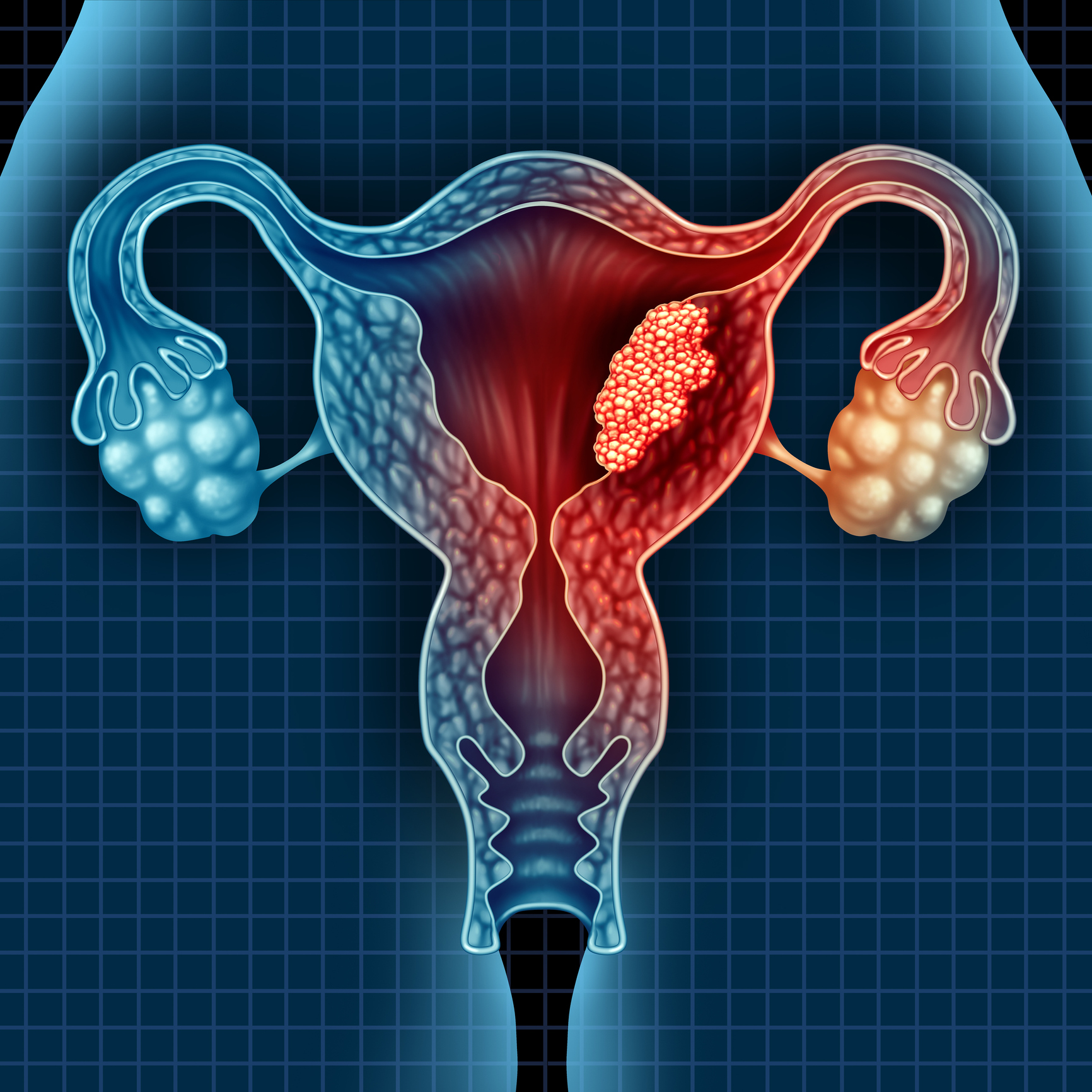
The uterus is an organ that involves in the reproductive functions in women. It is a pear-shaped organ containing four segments: fundus, corpus, cervix and the internal orifice of the uterus (also called internal os). The uterus has a pair of tubular extensions called horns that debouch to the fallopian tubes, leading to the ovaries. Its internal cavity is lined by a mucous membrane called endometrium. The first part of the menstrual cycle is devoted to thickening of the uterine lining for pregnancy. If fertilization occurs, the egg cell (ovum) will migrate from the fallopian tubes and make its implantation in the superficial layers of the endometrium to begin its embryonic development. If no fertilization occurs, the uterine lining is shed during menstruation.
Uterine cancer Statistics
Uterine cancer is one of the most common cancer of the female genital tract; it affects nearly 45 women per 100 000, mostly women who had never been pregnant. Each year, about 500,000 women are diagnosed with uterine cancer worldwide; the tumor represents approximately 13% of all cancers in women.
In the United States alone, approximately 40,000 women are diagnosed with uterine cancer each year. According to the American Cancer Society, it is estimated that 42,160 women were diagnosed with cancer of the uterine corpus in the US in 2009; about 7,780 women died of the disease.
Uterine Cancer Causes
The inside of the uterus is covered with a layer of cells called endometrium. At the beginning of each menstrual cycle, the endometrium thickens to possibly host an embryo at implantation. If at the end of the menstrual cycle, no embryo implants, much of the uterine lining peels off, thus constituting the menstrual period.
Unfortunately, sometimes due to environmental, chemical or physical factors, or certain viruses, certain cells lining the inside of the uterus multiply without control, and form cancerous growth. In another words, you have cancer of the uterus when DNA gene of a group of cells that line the inner of your uterus is damaged or changed in such a way that they reproduce anarchically to form a malignant growth.
Estrogen levels play a major role in the development of uterine cancer. Although several factors may influence the increased estrogen levels, obesity and menopause are the two major causative factors. There is no strong relationship between uterine cancer and STDs. The cancer can occur in women who have never had any sexual intercourse or HPV infection. Uterine cancer is more common among women who had few or no children.
Uterine Cancer Risk Factors
The most common factors that can increase your risk of developing uterine cancer include:
- Age – the average age of uterine cancer patients is 61 years with a majority of cases lie between 50 and 69 years. 5% of cancers are diagnosed before 40 years, 25% before menopause. Therefore, women over 50 are more at risk of uterine cancer.
- Race – uterine cancer is more common among white women living in Western countries.
- Infertility – if you have never had children, you are three to eight times more likely to develop uterine cancer compared to women who had children.
- High estrogen levels – cancer of the uterus is hormone-dependent tumor; its growth is favored by high estrogen hormone levels in the blood.
- Certain diseases – certain medical conditions such as diabetes, hypertension, under active thyroid and disorder of the gallbladder increase the risk of developing cancer of the uterus.
- Endometrial disease – if you have endometrial hyperplasia, your chance to have an increased risk to have cancer of the uterus.
- Family history – If you have a family history of uterine cancer or colon cancer, you are at greater risk.
- Obesity/Overweight – Your body produces some of its estrogen in fatty tissue; therefore, obesity or excess weight can cause a higher rate of estrogen, which may contribute to the occurrence of uterine cancer.
- Estrogen-only replacement therapy (ERT) – hormone therapy consists of estrogen without progesterone increases the risk of developing cancer of the uterus in a ratio of approximately 120% for each period of five years of use. However, when estrogen is associated with progesterone, the therapy is safe.
- Early first menstruation or late menopause – if you had your first menstruation at a young age (before age 12 for instance) and going through menopause at a late age, you are at greater risk of suffering from uterine cancer.
- Physical inactivity – sedentary lifestyle is the enemy of your body. It causes excess weight, cardiovascular problems, and much more. Regular Physical activity (including domestic work and fast walking), in the other hand, control the production of estrogen produced by the ovaries and reduce the risk of uterine cancer.
- Certain Medications – If you have been treated with tamoxifen to prevent or treat breast cancer, you are twice as likely to have cancer of the uterus.
- Fatty foods – in addition of cervical cancer, fatty foods and red meat are likely to cause many cancers.

Uterine Cancer Symptoms
In postmenopausal women, early symptom of uterine cancer is often bleeding or unusual vaginal discharge. While other health problems can lead to abnormal vaginal bleeding, for postmenopausal women, it is a red flag. Therefore, if you are menopausal woman and experience vaginal bleeding, consult your gynecologist immediately.
Fortunately, unlike many other cancers, symptoms of uterine cancer typically manifest in early stage of the disease. Therefore, the 5-year survival rate for uterinecancer is high.
In general, if you have cancer of the uterus, you will experience at least one of these symptoms:
- abnormal weight loss
- bleeding after menopause
- vaginal discharge
- bleeding between periods (premenopausal women)
- difficult or painful miction
- painfulsexual intercourse
- Pelvic pain, back pain and sometimes leg pain.
Uterine Cancer Complications
Cancer of the uterus diagnosed and treated early rarely causes complications; in fact, five-year survival rates are 95 percent when the tumor diagnosed at an early stage. However, late diagnosis does not perform well. A uterine cancer detected at an advanced stage can spread into other parts of the body to form other cancers (metastases). In this case, the cancer is more difficult to be treated, and survival chance is low.
Uterine Cancer Diagnosis
Your doctor will question you about your medical history and the symptoms you experience. In addition, he will do a physical examination of your abdomen and pelvis to look for signs indicating uterine cancer. However, these diagnostic steps can give him a suspicion of the cancer but not a confirmation.
For women who are closed to menopause and still have their menstruation, the diagnosis is more difficult; the bleeding can be a menorrhagia (abnormally heavy and prolonged menstrual period) or bleeding of a cause that has nothing to do with cancer. To rule out these non-cancerous bleeding, your doctor will do a direct pelvic examination – with a speculum- to assess your pelvic organs and check for any gynecological problems. In the absence of cancer, the test usually shows a normal cervix.
However, to confirm with certainty the presence of a uterine cancer, your doctor will recommend the following tests:
Pap test (Pap smear) – this test is done to look inside the vagina and the outside of the uterus. Your physician introduces a speculum into your vagina to take sample of cells from the cervix. A Pap test cannot reveal a uterine cancer; it is, however, a key technique to detect precancerous sign and prevent cancer of the pelvic organs.
Transvaginal ultrasound – this medical technique is painless; it consists of inserting two or three inches from the tip of a transducer into your vagina to obtain images of the uterus. This test allows your doctor to create images from different angles to get the best views of your uterus and ovaries. If any cancerous lesion is found on the endometrium, a biopsy will be performed.
Biopsy – even if the other procedures have revealed the cancer, a biopsy is usually necessary to establish with certainty the diagnosis. During the procedure, your doctor removes a small sample of tissue from the inside of the uterus for laboratory analysis. If cancer cells are found, other techniques will be performed to determine the stage of the cancer. In general, at least one of these biopsies will be performed.
- Endometrial biopsy – during this diagnostic procedure, your doctor introduces a thin, flexible tube through the cervix. He then uses a gentle suction to collect sample of tissue from the lining of the uterus. The biopsy may be performed in a hospital or at your doctor’s office.
Although rare, an endometrial biopsy may cause complications such as infections, bleeding or uterine perforation. If you experience pain or bleeding after the biopsy, call your doctor immediately.
- Dilatation and curettage – this is diagnostic technique allows your surgeon to evacuate or gradually open your cervix. Performed under local or general anesthesia, dilation and curettage allows your doctor to scrape the lining of the uterus to collect tissue sample for laboratory analysis.
Dilatation and curettage often causes pain similar to menstrual cramps a day or two after the procedure. If these problems persist for three or four days, see your doctor; it may be a sign of complications.
- Laparotomy – laparotomy is a surgical procedure consists of opening the abdomen through an incision so that the surgeon can have direct passage on the abdominal and pelvic organs. Performed under general anesthesia, laparotomy allows your surgeon to visually inspect and evaluate the tumor, surrounding tissue and lymph nodes. Laparotomy can also measure the extent of the tumor and whether it has spread or not.
Hormone Test
Although rarely performed before the treatment, your doctor may recommend hormonal testing to see whether estrogen receptors are present in the tissue of the tumor. A positive result indicates that hormone therapy can have a positive effect against the cancer.
Uterine Cancer Stages
After confirming the diagnosis, a series of tests will be done to determine the stage of the cancer. In general, the stages of uterine cancer include:
- Stage I – the cancer is localized only in the uterus; it has not spread.
- Stage II – the cancer has affected both your uterus and cervix, but has not crossed the Pelvis.
- Stage III – at stage 3, the cancer has spread outside the uterus to reach other organs such as lymph nodes housed in the lower abdomen (pelvis), but has localized in the pelvic area.
- Stage IV – Stage IV is the most advanced stage of uterine cancer; the cancer has spread to the upper abdomen and may affect the bladder, rectum or other remote parts of your organism.
- Recurrent – a cancer that has returned after treatment is considered as a recurrent cancer. In general, recurrent uterine cancers are more difficult to be treated.
Uterine Cancer Treatment
Uterus cancer treatment consists mainly of two local therapies: surgical therapy and radiotherapy, and two systematic therapies that affect your entire organism: hormone therapy and chemotherapy.
Your doctor will use at least one of the basic treatments (surgery, radiotherapy, hormone therapy and chemotherapy) to combat the cancer. However, treatment used depends on your age, health status, location and stage of the cancer. Your health care provider may use a combination of these treatments to increase your chance of recovery.
Surgical treatment
Surgery is considered as the essential treatment of uterine cancer; it is fairly the safest method to completely eliminate the cancer. Depending on the stage of the cancer, your surgeon may perform a hysterectomy, removal of part or the entire uterus; or a hysterectomy with bilateral salpingo-oophorectomy, removal of the uterus along with the vagina, cervix, fallopian tubes and ovaries.
This is usually done through an incision in the abdomen, under general anesthesia; the surgery requires hospital stay. Although this method is new and less common, some surgeons have begun using the laparoscope for the detachment of the fallopian tubes and ovaries to complete the hysterectomy vaginally.
Whatever the method used to perform the hysterectomy, you will not be able to get pregnant after your uterus has been removed; talk to your surgeon if you plan to get pregnant in the future.
For a stage I uterine cancer, surgery is sometimes the only treatment necessary. In advanced or metastatic uterine cancer, however, chemotherapy, radiotherapy or hormone therapy can be associated.
Radiation Therapy (radiotherapy)
Treatment of a uterine cancer diagnosed at stage II, III or IV, surgery must be followed by radiation therapy to destroy locally the cancerous cells and reduce the risk of recurrence or metastasis. In rare cases, however, radiotherapy can be administered before surgery in order to reduce the size of the tumor to facilitate its excision. Whether performed before or after the surgery, internal or external radiotherapy will be used. In some cases, both methods can be practiced.
- External beam radiation therapy – this method involves projecting high-dose of X-rays to the tumor to kill cancer cells. External radiation therapy is usually administered on an outpatient basis, once a day, and five days a week for several weeks.
- Internal Radiotherapy – during this procedure, small tube containing radioactive material are inserted into your vagina for several hours to several days. The internal radiation therapy always requires hospitalization.
Chemotherapy
Chemotherapy involves the use of powerful chemical agents (drugs) to kill cancer cells. Chemotherapy is used to treat uterine cancer if the cancer is very aggressive (a cancer that spreads very quickly) or has spread beyond the uterine. Chemotherapy drugs can be taken by mouth, infusion or injection. In the treatment uterine cancer, however, chemotherapy drugs are usually administered intravenously to navigate the bloodstream to reach all parts of the body. Your doctor may administer several medications (polychemotherapy) at the same time to facilitate the destruction of the cancerous cells.
However, the chemotherapy drugs attack both the tumor cells and normal cells, which can cause side effects. Side effects vary from one person to another, from one drug to another. Most common adverse effects of chemotherapy medications used to treat uterine cancer include:
- nausea
- low blood cells count
- stomach pain
- vomiting
- loss of appetite
- temporary hair loss
- increased vulnerability to infections
- Fatigue.
Hormone therapy
Hormone therapy usually involves taking synthetic progestin pills or gonadotropin-releasing hormone agonists (GnRH agonist) to stop the proliferation of the cancer cells. Hormone Therapy is most often used to treat advanced or recurrent uterine cancers.
Uterine Cancer Survival Rates
Unlike many other cancers, uterine cancer has a good prognosis. The fact that it is often diagnosed early, uterine cancer is often successfully removed surgically. However, the survival rates tend to vary by race. The overall 5-year relative survival rate for 1999-2005 was 82.9%. Five-year relative survival rates by race were:
84.7% for white women
61.3% for black women.
Uterine Cancer Prevention
Development of uterine cancer is not due to one cause, several factors are suspected in its occurrence. Some risk factors such as age, menopause is impossible to change, others can be successfully prevented. The following preventive measure can help you reduce your risk of uterine cancer:
Stop smoking – in addition to uterine cancer, cigarette smoke can also increase the risk of the following cancer:
- kidney cancer
- bladder cancer
- lung cancer
- colon and rectum cancers
- cervical cancer
- esophageal cancer
- laryngeal cancer
- oral cavity / throat cancers
- pancreas cancer
- stomach cancer
- and more.
Adopting a healthy diet – there is an increased risk of uterine cancer linked to consumption of saturated fat, especially animal fats and fried foods. In the other hand, a high intake of fruits, cruciferous vegetables and cereals (especially those that are high in beta-carotene) helps reduce the risk of many cancers, including uterine cancer.
Exercise regularly – many studies have shown that regular physical activities such as fast walking and activities performed as recreation reduce the risk of several types of cancer including uterine cancer after menopause.
Maintain a healthy weight – many studies have shown that being overweight plays a role in the development of all cancers. A Dutch epidemiological research that followed 25 000 women aged 40 to 65 years over 13 years found that overweight in postmenopausal women was one of the two main risk factors for uterine cancer and endometrial hyperplasia.
Limit intake of estrogen – if you are obligated to take hormone therapy for menopause symptoms, it is recommended that the medication contains progesterone to counteract the negative effect of estrogen.
Limit your alcohol intake – moderate alcohol consumption poses no risk of cancer; heavy consumption, in the other hand, is a major causative factor.