Table of Contents
Atherosclerosis
You have atherosclerosis when the inner lining (intima) of your arteries are clogged with plaques of atheroma, a fatty deposit formed of cholesterol, cell debris and fatty acids. Atherosclerosis involves primarily the thickening of the wall of large arteries such as abdominal aorta, coronary arteries, cerebral arteries and arteries of the legs.
The risk of atherosclerosis increases with age. That is, as you get older, the tissues of the arteries lose their elasticity and become stiffer. This disorder causes an obstacle to the blood flow and makes it difficult the passage of oxygen and other nutrients such as LDL cholesterol (the major cholesterol carrier in the blood). Thus, atherosclerosis is not a sudden illness, but a progressive arterial disorder. Although the disease can be due to many causative factors, obesity and diet are the two main causes.
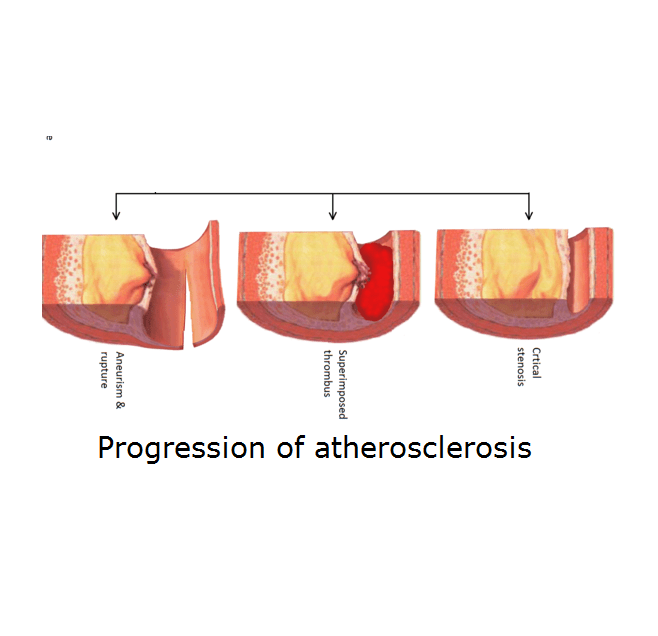
Atherosclerosis is a progressive disease; it can start asymptomatically very early in life and waiting until age 20 to produce minor symptoms, which are often negligible. At the age of 40, however, the atherosclerotic plaque developed in the arteries tends to be become harder and larger which makes the symptoms manifest painfully. At this point, your risk of developing cardiovascular disease is high; you do need medical treatment to prevent complications.
A little history of atherosclerosis
The term atherosclerosis was first introduced in 1904 by Felix Marchand. He composed atherosclerosis from two Greek words “ather” which means boiled and “skleros” which means hard. In 1958, The World Health Organization (WHO) described atherosclerosis as an accumulation of fats (lipids), complex carbohydrates (sugars), blood and blood products, fibrous tissue and calcium deposits on the inner layer of large and medium arteries.
Until today, the term atherosclerosis is still used in the medical elite. The disease is one of the first causes of mortality in developed countries and particularly countries of Europe and North America.
Atherosclerosis Causes
Atherosclerosis is a multifactorial disease; it can be due to genetic, lifestyle and environmental factors that act synergistically to promote its development. Atherosclerosis is a life threatening condition; it is responsible for the leading cause of death in the industrialized countries, heart disease.
The most common factors suspected in the development of atherosclerosis included:
Age – the older you get, the higher your risk of developing atherosclerosis. With age the plaques are formed and organized in your arteries wall, making the arteries hard and nondistensible (lose their capability to stretch and expand). The arteries can clog and break, which can lead to stroke or heart attack.
Sex – although atherosclerosis does not make acceptation of sex, it is more common in men. It can affect men from age thirty five. In women, however, it is more frequent after menopause. The reason is that before menopause, women blood tends to be less rich in cholesterol.
Foods – foods rich in sugar and cholesterol is the enemy of your cardiovascular system. You organism needs cholesterol to function properly; cholesterol is used by your body to build cell membranes and produce certain hormones. It is through the degradation of cholesterol that the liver receives the bile acids used in digestion of fats in the intestine. However, excess cholesterol is the primary cause of atherosclerosis. In other words, your body needs cholesterol but at a normal levels.
Obesity – atherosclerosis is frequently associated with obesity. Medical studies conducted on arteries taken from adults aged 15 to 34 years died accidentally show that obese patients present plaques of diffuse and complex atheroma in the arteries of their heart and aorta. Obesity is associated with all other cardiovascular problems, including cardiac arrest. In addition, the risk of certain types of cancer seems to be higher in people who have excess body weight.
Tobacco – besides multiple types of cancer that it can cause, tobacco is a deadly substance for your cardiovascular tissues. Tobacco in all its forms (chewing, smoke, and second hand smoke) plays an important role in the increase of bad cholesterol (LDL). In other words, the more you smoke, the higher is your LDL; high levels of LDL equal increased risk of atherosclerosis.
Hypertension – this cardiovascular disorder is one of the main factors for atherosclerosis. Hypertension acts by damaging the artery wall and thereby creates small lesion. Without interruption, along with cholesterol, blood cells debris will stick into the breach, leading to the formation of atherosclerotic plaque.
Certain illnesses – some illnesses such as diabetes may increase the levels of cholesterol, sugar and insulin in your blood, and promote the development of atherosclerotic plaques. However, the relationship between diabetes and atherosclerosis is relatively complex for scientists.
Atherosclerosis is very common among individuals with gout (hyperuricemia). Since gout and high cholesterol are often the result of bad eating habits, scientists believe that the problem is the result of an unhealthy lifestyle.
Stress – after numerous researches, no one can doubt that stress is the root of many diseases that ravage our planet. Stress plays a role in the development of atherosclerosis by releasing adrenaline, which in turn causes spasms in the arteries. When this problem happens too often, it can cause high blood pressure (hypertension) and repeated arterial spasms and thus promoting atherosclerosis.
Sedentary – your body needs to be active for the proper functioning of the muscles, cardiovascular system and all the other systems in your organism including the immune system. Lack of physical activity increases the levels of LDL, decreases the resistance of the arteries and promote the development of cardiovascular disease. Exercise, in the other hand, increases the rate of “good cholesterol” and strengthens the immune system. At least 4 times a week, it is recommended to walk, swim, or jog. Reducing your physical inactivity is the most effective way to prevent or slow the progression of atherosclerosis.
Atherosclerosis Warning Signs and Symptoms
You may have atherosclerosis for years without developing any symptoms. In most patients, signs and symptoms tend to appear at ages 40-50; in some individuals, atherosclerosis symptoms can even take longer than that to manifest. In general, atherosclerosis symptoms start emerging when the obstruction has reached 70 and 80% of the artery wall, causing the cells and organs to be deprived of normal amount of oxygen needed to function well. Atherosclerosis symptoms vary greatly depending on the organ affected; therefore:
- Located in a coronary artery, atherosclerosis is characterized by angina pectoris (angina) and myocardial infarction;
- When the cerebral arteries are affected, stroke can occur due to obstruction of one or more arteries supplying the brain;
- If the aorta is affected, aortic aneurysm or aortic dissection can occur
- An atherosclerosis of the arteries of the lower limbs can lead to pain and arthritis of the legs
- Atherosclerosis of renal artery usually causes renal hypertension.
Complications
Atherosclerosis can lead to complications and even death. If you smoke or have high cholesterol, your risk is even greater. Consult your doctor immediately if you experience chest pain during exercise or leg pain with walking. This may be a sign of angina pectoris or evolution of arthritis of the lower limbs. In addition, consult your doctor if you experience a decrease in muscle strength of a limb or hand, or a sudden problem of vision or speech. This may indicate a blockage of a cerebral artery, the major cause of stoke
Diagnosis
In general, your doctor will do a physical examination to detect signs indicating an atherosclerosis. He will look for weak pulse, low blood pressure in an affected limb and signs of aneurysm. In addition, with a stethoscope, your cardiologist will listen to your heart beat for an abnormal whooshing sound. Usually, those suspicious signs are not enough to confirm the diagnosis, other procedures such as blood tests, angiogram, Doppler ultrasound, ankle-brachial index test, and magnetic resonance angiogram (MRA) can be recommended.
Blood test – a blood test is often important in the diagnosis of atherosclerosis; it allows your doctor to determine your blood cholesterol level and other indices important in the diagnosis.
Doppler ultrasound – Doppler examination is a painless procedure based on the use of ultrasound (sound waves). It helps your physician locate and measure the arterial plaque. This technique is very effective and it can detect atherosclerosis before signs and symptoms emerge.
Coronary angiography – this imaging technique helps your oncologist visualize your blood vessels or chambers of the heart. During the procedure, the specialist injects a contrast agent intravenously or directly into your femoral artery to facilitate the visualization. Arteriography is more complex than the Doppler exam and it sometimes requires hospitalization for about a day.
Ankle Brachial Pressure Index (ABPI) – this is a medical technique used to compare blood pressure in your legs with blood pressure in your arms. Compared to the arm, lower blood pressure in the leg is a symptom of blocked arteries, a vivid sign of atherosclerosis.
Electrocardiogram (ECG) – this radiographic examination consists of recording the electrical impulses of the heart. During the exam, the technician will place small electrodes on your chest and connect them to an electrocardiograph. During the procedure, your cardiologist will be able to determine the form and severity of the atherosclerosis. Since the symptoms of atherosclerosis do not usually occur in the hospital, you may be recommended to continue the exam at home by using portable ECG devices. Whenever possible, the ECG should be done during the atherosclerosis attack.
Computed tomography angiography (CTA) – your health care provider can perform this exam to visualize arterial and venous vessels throughout your body. Your doctor can recommend a CTA to detect narrowing of blood vessels in many areas of your body, including brain, kidneys, pelvis, and the lungs. This method is the ideal choice for diagnosing arterial disease; it is safer and much less time-consuming than other imaging techniques including catheter angiography.
Atherosclerosis Treatment
Atherosclerosis can be treated with medications or surgery.
Drug treatment
Usually, your doctor will recommend you to follow a method capable of restoring the health of your arteries. If exercise and proper diet is not enough to normalize your cholesterol levels and unblock the arteries, you will be prescribed drugs such as fibrates, statins and cholestyramine (Questran).
To reduce blood clot formation, you can take anti-platelet medications and blood thinners such as aspirin, heparin or warfarin. Atherosclerosis is often accompanied with hypertension; your doctor may recommend you to take beta blockers, angiotensin-converting enzyme (ACE) inhibitors and calcium channel blockers to keep your blood pressure in normal range.
Injection
Thrombolytic drugs injection – thrombolytic therapy is a simple procedure, during which special drugs are used to clear a blocked artery; this prevent damage that may be caused by the blockage of the blood vessel.
Surgical Treatment
In case of complications where the arteries are severely blocked, medications are not ineffective; you need one of the following surgeries:
Angioplasty – Angioplasty is a surgical technique used to modify a blood vessel, usually an artery. During the procedure, your surgeon uses small inflatable balloons that can dilate the artery where it is obstructed to restore normal blood flow. In most cases, the intervention is completed by the introduction of a metal prosthesis (stent or spring) which is embedded inside the vessel to prevent re-narrowing.
Angioplasty can be performed without the surgical intervention. Depending on the characteristic of the disease, your health care provider can perform a needle puncture of the vessel or percutaneous coronary intervention (PCI). Whatever method used, you will be recommended to take drugs for a long period of time after the angioplasty.
Endarterectomy – If you have atheromatous plaque material, or blockage, in the lining of an artery, an endarterectomy can be performed to remove those pathological deposits. This surgical procedure can also be used as a supplement to a vein bypass graft to open up distal segments.
Bypass Surgery– obstruction of a coronary artery can prevent normal circulation of blood reaching the heart muscle. When blood flow is reduced, it can result in angina pectoris or even heart attack. A bypass surgery consists of installing a graft between the aorta and the coronary artery to restore normal blood flow in a narrowed or obstructed artery.
Alternative Remedies
Drink pomegranate juice several times daily; many studies have shown pomegranate reduces the risk of developing atherosclerosis. Along with the pomegranate, increase the following vitamins and minerals in your diet:
- Vitamin C
- Vitamin E
- Vitamin D
- proline
- Lysine
- Folic acid
- Biotin
- Copper
- Chondroitin sulfate
- N-acetylglycosamine.
Atherosclerosis Prevention
The key to prevent atherosclerosis and all other cardiovascular disease is excising regularly, losing weight (if you are obese or overweight) and stopping smoking (including second hand smoke). In addition, you need to consume a healthy diet:
- Increase your intake of antioxidants
- Avoid saturated acids, mainly from animal fats, pastries, margarine, etc.
- Increase your intake of carbohydrates and fiber; they play an important role in increasing the levels of good cholesterol
- Reduce bad cholesterol: egg yolk, organ meats (brain, kidney, liver), nuts, almonds, lobster, shellfish, fish eggs, etc.
- Consuming polyunsaturated fatty acids such as omega-6 (sunflower oil) omega 3 (flax seed oil, fish oil), they lower the bad LDL cholesterol and prevent the formation of a blood clot.
- Eat plenty fruits (2 to 3 per day), vegetables (3 to 4 servings per day), polyphenols (moderate consumption of wine and green tea) and phyto-oestrogens: soy, green tea, chickpeas, lentils, beans, grains, carrots, fennel, onions, garlic, etc.
References:
1 – Berchtold, P., Jorgens, V., Finke, C., and Berger, M.: Epidemiology of obesity and hypertension. Int. J. Obes. 1981; 5(Suppl. 1):1
2 – M. Aviram, N. Volkova, R. Coleman, M. Dreher, M. Kesava Reddy, D. Ferreira, M. Rosenblat “Pomegranate Phenolics from the Peels, Arils, and Flowers Are Antiatherogenic: Studies in Vivo in Atherosclerotic Apolipoprotein E-Deficient (E0) Mice and in Vitro in Cultured Macrophages and Lipoproteins” Journal of Agricultural and Food Chemistry Published on-line ahead of print, ASAP Article, doi: 10.1021/jf071811q
3 – Denke, M. A., Sempos, C. T., and Grundy, S. M.: Excess body weight: An underrecognized contributor to high blood cholesterol levels in white American men. Arch. Intern. Med. 1993; 153:1093,
3 – Eckel RH, Krauss RM. American Heart Association call to action : obesity as a major risk factor for coronary heart disease. AHA Nutrition committee. Circulation 1998; 97: 2099-100
4 – Le cholestérol n’a rien à voir avec le développement de l’athérosclérose
5 – Garrison, R. J., Wilson, P. W., Castelli, W. P., et al.: Obesity and lipoprotein cholesterol in the Framingham Offspring Study. Metabolism 1980; 29:1053
7 – Hartz, A. J., Rupley, D. C., Kalkhoff, R. D., and Rimm, A. A.: Relationship of obesity to diabetes: Influence of obesity level and body fat distribution. Prev. Med. 1983; 12:351
8 – Pourquoi les animaux n’ont pas d’attaque cardiaque…mais les hommes si! Partie 1
9 – Hubert HB, Feinleib M, McNamara PM, Castelli P. Obesity as an independent risk factor for cardiovascular disease : a 26-year follow-up of participants in the Framingham heart study. Circulation 1983 ; 67 : 968-77
10 – Pourquoi les animaux n’ont pas d’attaque cardiaque…mais les hommes si! Partie 2
11 – Thompson, Jesse E., The Evolution of Surgery for the Treatment and Prevention of Stroke
12 – “Health Information—Find Articles, Tools, and Tips at MerckEngage.com”. ww.mercksource.com .
13 – Dobarganes C, Márquez-Ruiz G (2003). “Oxidized fats in foods”. Current Opinion in Clinical Nutrition and Metabolic Care 6 (2): 157–63. doi:10.1097/00075197-200303000-00004. PMID 12589185.
14 – supplements, FDA. “Dietary Supplements”.
15 – Chih-Hao Wang. “Biological Gradient Between Long-Term Arsenic Exposure and Carotid Atherosclerosis”. www.ahajournals.org
16 – Downs JR, Clearfield M, Weis S; et al. (May 1998). “Primary prevention of acute coronary events with lovastatin in men and women with average cholesterol levels: results of AFCAPS/TexCAPS. Air Force/Texas Coronary Atherosclerosis Prevention Study”. JAMA: the Journal of the American Medical Association 279 (20): 1615–22. doi:10.1001/jama.279.20.1615. PMID 9613910.