Table of Contents
Atrial Fibrillation
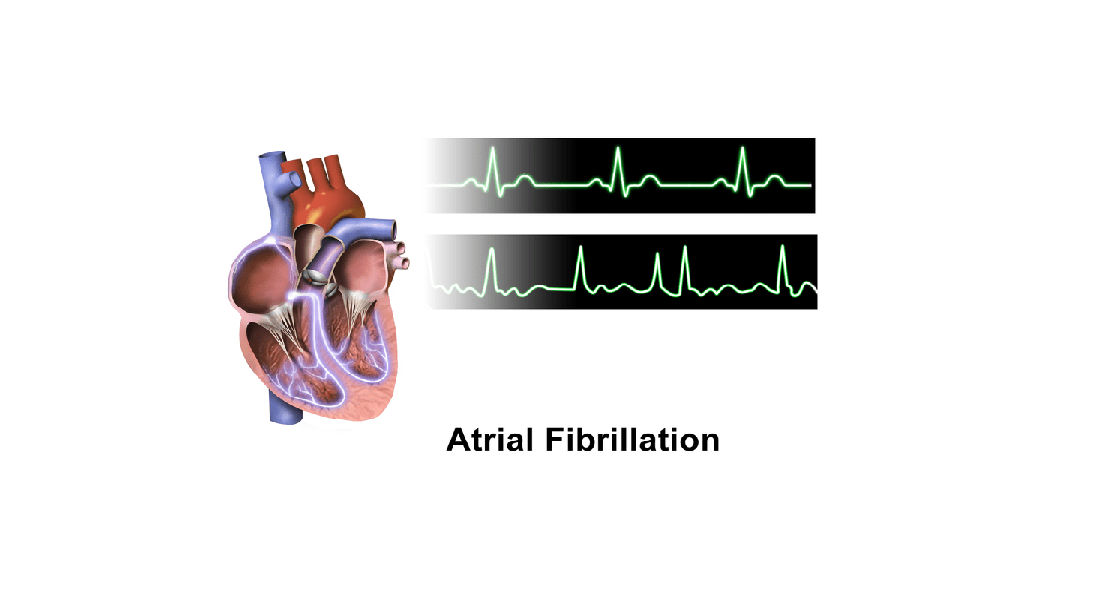
Atrial fibrillation is a rapid and irregular contraction of the two upper chambers of the heart muscle (atria) due to uncoordinated action of the atrial cells. In other words, if you have atrial fibrillation, your heart rate becomes rapid and irregular. Atrial fibrillation is considered permanent when persisting for more than a year, persistent if it lasts for at least 7 days, and paroxysms when it takes less than 7 days.
Your heart has four chambers: two atria, which are the two upper two chambers of the heart, and two ventricles, the lower two chambers. As the heart muscle contracts, it pumps blood out of the heart into other parts of the body. The normal cardiac contraction is made by a cyclic depolarization (reversing the electric polarity of the cell membrane) of a group of cells on the upper right atrium called “sinus node”. This depolarization propagates downward toward the atrioventricular node, a small group of cells that connect the atrial and ventricular chambers electrically. In the case of atrial fibrillation, depolarization becomes chaotic causing an uncontrolled contraction of the atria, and rapid and irregular contraction of the ventricles.
Atrial fibrillation is the most common form of cardiac arrhythmia; it affects approximately 1% of the world population, with an incidence of almost 5% in the population over 65 years and about 10% in people aged over 80.
Atrial Fibrillation Symptoms
In certain patients, atrial fibrillation can be totally asymptomatic at the beginning. Most of the times, atrial fibrillation is discovered during an examination done for another medical condition.
When symptoms finally occur, they tend to vary from person to person. The characteristics of atrial fibrillation symptoms you experience also depend on the type of fibrillation you have. For instance, if you have paroxysmal atrial fibrillation, you may experience a sudden heartbeat, which can last several minutes to several days. In permanent or persistent atrial fibrillation, you may have painless palpitations that can be more or less tolerated. Permanent atrial fibrillation can also lead to fatigue or a moderate dyspnea. In general, if you have atrial fibrillation, you will experience at least one of these symptoms:
- Weakness
- Dizziness
- Shortness of breath
- Chest pain
- Irregular palpitations
- Feeling of anxiety
- Decreased blood pressure
- Irregular heartbeat and rapid up 500/minutes
- Lightheadedness accompanied by fainting.
Complications
Atrial fibrillation can be effectively controlled by medical treatment (medication, surgery or both), but its tendency to develop multiple complications makes it a life threatening disease. Untreated atrial fibrillation can lead to serious medical problems. The most common complications of atrial fibrillation include:
- Recurrence
- Heart failure
- Double the risk of cardiovascular mortality
- Ventricular fibrillation and sudden death
- Increased to adverse effects or complications related to medical treatments (iatrogenic)
- thromboembolic events – the risk of stroke is 5 times higher in patients with atrial fibrillation
- Development of atrial ectopic rhythm (the atria do not beat in harmony with the ventricles)associated with hyperexcitability and bradycardia (slow heartbeat).
None of those symptoms should be neglected; they can be signs of serious medical conditions such as stroke and heart attack. Contact your health care provider immediately if you have abnormal heart beats accompanied with chest pain. If you are unable to contact a health care specialist, it would be wise to call 911.
Atrial Fibrillation Causes
Atrial fibrillation is characterized by cardiac arrhythmias. Its causes are not always known, but scientists believe that age is the basic factor favoring its occurrence; atrial fibrillation is present mainly in the elderly. In general, high levels of catecholamine and thyroxine in the atrial fibers and dilatation of the left atrium promote its formation and evolution.
Factors leading to atrial fibrillation may be cardiac or extracardiac.
Most common cardiac factors include:
- Coronary disease
- High blood pressure (cardiovascular factor)
- Disease of the atrium
- Hypertrophy of the left ventricles
- Disorders of the mitral valve (rheumatic and non-rheumatic)
- Previous heart surgery
Less frequent cardiac factors include:
- dilated or hypertrophic cardiomyopathy
- pericarditis
- Heart attack
- atrial myxoma embolism
- pulmonary heart disease
- congenital heart disease such as atrial septal defect (ASD).
Extra-cardiac factors:
- Hyperthyroidism
- Infection
- Diabetes
- Sleep apnea
- Chronic alcoholism
- Viral infection
- Lung diseases such as emphysema and pneumonia
- Use of caffeine, tobacco, alcohol or certain medications.
Diagnosis
Usually, your cardiologist will ask you questions about your medical history and make a physical examination to detect signs indicating an atrial fibrillation. Usually, these signs will be detected by cardiac auscultation: fast or irregular heartbeat, heart murmur, etc. Your physician will also look for high blood pressure, and signs of hyperthyroidism, pulmonary embolism and pericardial friction rub (audible medical sign of pericarditis).
Physical examination alone is not sufficient to confirm an atrial fibrillation diagnosis; your doctor will recommend other medical techniques that are more specific:
Electrocardiography (ECG) – this test is quick, painless, and noninvasive. It causes no health problems, and only takes a few minutes to be performed. An ECG can be done in doctor’s office, hospital or at home. The electrocardiogram can show graphically the electric potential controlling the activity of the heart muscle. Using a medical scope, the result is displayed on a screen, which allows your doctor to determine if the electrical activity of your heart muscle is normal or not.
Echocardiography – this is an imaging technique consist of using sound waves (ultrasound) to examine the heart muscle. An echocardiography allows your cardiologist to view the size and shape of your heart and the functioning of the cardiac chambers and valves. Echo exam is commonly used in the diagnosis of atrial fibrillation to:
- detect heart failure
- study heart valves, mainly in search of abnormalities of the mitral valve
- study the cardiac chambers, in search of left ventricular hypertrophy (LVH), thrombus in the left atrium, atrial dilation, etc..
Blood test – your doctor may recommend a blood test to look for hyperthyroidism evidence. This test will be done if thyroid problems are suspected.
Chest x-ray – a chest radiograph is important to determine your heart size and search for vascular overload, which can indicate a heart failure.
Holter monitor – this is a portable medical device allowing you to continuously monitoring your heart function for hours or days. The device will be connected by electrodes attached to your skin by adhesive. Also, this diagnostic machine has a button which you can activate if you feel any pathological signs: palpitations, chest pain, irregular heartbeat, etc. In addition, there is a marker placed on the recorder allowing you to note all the diagnostic details your doctor needs for the diagnosis.
Event monitor – in case you have a persistent dysrhythmia, you may be recommended to carry a cardiac event monitor; this allows your doctor to have a better idea of your abnormal heart rhythms, and take further therapeutic action if necessary. Event monitor allows you to records your heart’s electrical rhythm while you are at home, which will be reviewed by your health care provider during visit.
Atrial Fibrillation Treatment
As with any disease of the cardiovascular system, a change of lifestyle is important during and after atrial fibrillation treatment. Therefore, it is important to stop smoking, practice regular physical activity and adopt a heart healthy diet. Avoidance of certain stimulants such as caffeine and alcohol is also necessary. In addition, it is important to continue the treatment, even in the absence of symptoms.
The goal of the treatment is to stop the atrial fibrillation so that the heart muscle can restarts beating normally. Therefore, atrial fibrillation treatment consists of four phases: Normalize the heartbeat, keep the normal heart rhythm, control heart rate and prevent clotting in the left atrium.
Restoring the heartbeat
Your cardiologist can use two methods to restore your heart’s normal rhythm (sinus rhythm): taking medication or external shock therapy.
- Drugs – depending on the severity or symptoms of the disease, your doctor can prescribe you anti-arrhythmic drugs to help restore the normal rhythm of your heart. Those drugs can be taken orally or intravenously; and they are often taken after a couple weeks of taking blood-thinning medications. The most common anti-arrhythmics used in the treatment of atrial fibrillation include: amiodarone, flecainide and propafenone. Side effects may include: nausea, vomiting, heartburn, bloating, decreased appetite, stomach cramps, dizziness, drowsiness, weakness, headache, changes in sleep, muscle aches, sweating, dry mouth, tremors, and abnormal taste in the mouth. Although rare, you may also develop chest pain, blurred vision, unusual bleeding or bruising, skin rash, chills, sore throat, sudden weight gain, swelling of the ankles/feet, and trouble breathing.
- External shock therapy – also called cardioversion or defibrillation, external shock therapy is a medical procedure consisting in passing voluntarily and briefly an electrical current through the heart when involved in fibrillation to restore normal heart rhythm. Usually, external shock therapy is performed under anesthesia.
Keep the heart rhythm normal
After your sinus rhythm (normal rhythm) has been restored, your doctor will prescribe you antiarrhythmic drugs to take orally to help you maintain a normal heart rhythm. In general, you will be recommended to take at least one of these drugs amiodarone (Cordarone), propafenone (Rythmol), disopyramide (Norpace), sotalol (Betapace), flecainide (Tambocor) and quinidine (Quinaglute, Quinidex, Quinora). However, prescription of antiarrhythmic medications is not necessary in all case of atrial fibrillation. Talk to your doctor for more details.
Controlling the Heart Rate
If all attempts to restore a normal heart rhythm are unsuccessful, your cardiologist can content to slow the heart rate to prevent the onset of disabling symptoms and other complications related to atrial fibrillation. Slowing the arrhythmia would be more effective than trying to regulate the rate or prevent the recurrence of rhythm disorder.
Drugs used to correct atrial fibrillation and maintaining a normal sinus rhythm are especially beta-blockers, calcium antagonists bradycardia (diltiazem and verapamil) and digoxin. Most often, these drugs help to maintain the resting heart rate less than 80 beats per minute.
However, medications to control heart rate are not always effective. If unsuccessful, your doctor will perform a medical procedure called “AV node ablation” (atrioventricular node ablation). This is a sort of disconnection between the atria and ventricles of the heart by a technique of radio frequency that will destroy the “bundle of His”, a group of heart muscle cells specialized for electrical conduction that transmits the electrical impulses from the AV node (located between the atria and the ventricles) to the point of the apex of the fascicular branches. AV node ablation often brings good result; it requires, however, the establishment of a permanent pacemaker.
Prevent blood clotting in the left atrium
Your risk of having blood clot is higher when you have atrial fibrillation, therefore, during the treatment, prevention of the formation of thrombus in the atrium is very important. Your doctor may prescribe warfarin (Coumadin) or an anticoagulant treatment by heparin – standard intravenous or subcutaneous heparin or subcutaneous low–molecular–weight heparin (LMWH). Usually, this treatment is relayed by an anticoagulation using oral vitamin K. These drugs must be taken for at least 1 month and then discontinued if the arrhythmia is considered stable.
Atrial Fibrillation Prevention
The key to prevent all cardiovascular diseases including atrial fibrillation is excising regularly, losing weight (if you are obese or overweight) and stopping smoking (including second hand smoke). In addition, you need to consume a healthy diet.
- Increase your intake of antioxidants
- Avoid saturated fats, mainly fats from animal, pastries, margarine, etc.
- Increase your intake of carbohydrates and fiber; they play an important role in increasing the levels of good cholesterol
- Reduce bad cholesterol: egg yolk, organ meats (brain, kidney, liver), nuts, almonds, lobster, shellfish, fish eggs, etc.
- Consuming polyunsaturated fatty acids such as omega-6 (sunflower oil) omega 3 (flax seed oil, fish oil), they lower the bad LDL cholesterol and prevent the formation of a blood clot.
- Eat plenty fruits (2 to 3 per day), vegetables (3 to 4 servings per day), polyphenols (moderate consumption of wine and green tea) and phyto-oestrogens: soy, green tea, chickpeas, lentils, beans, grains, carrots, fennel, onions, garlic, etc.
References:
1 – Cayley W.E. Jr. Pharmacologic cardioversion for atrial fibrillation and flutter. Am Fam Physician 2005 ; 72 (11) : 2217-9.
2 – Furberg CD, Psaty BM, Manolio TA, Gardin JM, Smith VE, Rautaharju PM, Prevalence of atrial fibrillation in elderly subjects (the Cardiovascular Health Study) [archive], Am J Cardiol, 1994;74:236-241
3 – Miyasaka Y, Barnes ME, Gersh BJ et als. Secular trends in incidence of atrial fibrillation in Olmsted County, Minnesota, 1980 to 2000, and implications on the projections for future prevalence [archive], Circulation, 2006;114:119-125
4 – Mant J, Fitzmaurice DA, Hobbs FDR, et als. Accuracy of diagnosing atrial fibrillation on electrocardiogram by primary care practitioners and interpretative diagnostic software: analysis of data from screening for atrial fibrillation in the elderly (SAFE) trial [archive], BMJ, 2007;335:380-2
5 – Wolf PA, Abbott RD, Kannel WB, Atrial fibrillation as an independent risk factor for stroke: the Framingham Study [archive], Stroke, 1991;22:983-988
6 – The AFFIRM investigators, A comparison of rate control and rhythm control in patients with atrial fibrillation [archive], N Engl J Med, 2002; 34: 1825–1833
7 – Roy D, Talajic M, Nattel S et Als. [358:2667-2677 Rhythm control versus rate control for atrial fibrillation and heart failure], N Eng J Med, 2008;358:2667-2677
8 – Hart RG, Pearce LA, Aguilar MI, Meta-analysis: Antithrombotic Therapy to Prevent Stroke in Patients Who Have Nonvalvular Atrial Fibrillation, Ann Int Med, 2007:146:857-867
9 – The ACTIVE Investigators, Effect of clopidogrel added to aspirin in patients with atrial fibrillation [archive], N Engl J Med ,2009;360:2066-2078
10 – Haissaguerre M, Jais P, Shah DC et als. Spontaneous initiation of atrial fibrillation by ectopic beats originating in the pulmonary veins [archive], N Engl J Med, 1998;339:659-66
11 – http://en.wikipedia.org/wiki/Bundle_of_His