Table of Contents
Coronary Heart Disease
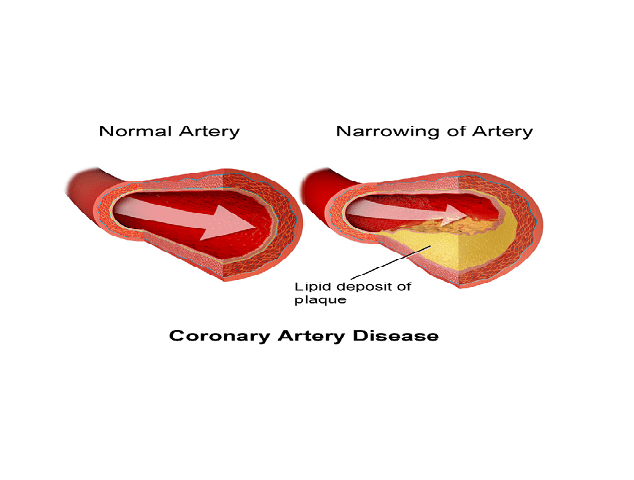
Coronary heart disease, also called coronary artery disease or coronary disease, is an obstruction within the coronary arteries due to formation and accumulation of fatty deposits. The coronary arteries are vessels that carry oxygen and nutrients to the heart muscle (myocardium). Build up of fats within their walls cause them to become narrowed or blocked, resulting in decreased oxygen or/and blood flow to the heart. If the heart is only starved of oxygen, angina (chest pain) and shortness of breath occur; if the artery is completely unable to pump blood to the myocardium, a heart attack occurs.
 Although coronary heart disease affects both sexes, it seems to cause more deaths among men; it is responsible for about 12.7% of total men deaths. In men, coronary disease tends to happen around age 45 to 64 years; while among women it occurs mostly around age 65.
Although coronary heart disease affects both sexes, it seems to cause more deaths among men; it is responsible for about 12.7% of total men deaths. In men, coronary disease tends to happen around age 45 to 64 years; while among women it occurs mostly around age 65.
However, many of these deaths could be prevented by reducing risk factors of the disease: unhealthy diet, hypertension, high cholesterol levels, smoking, obesity, physical inactivity, etc.
Statistics
Any blood circulation problem in the heart vessels is a serious matter; without an effective therapy, the heart will stop working properly or stop beating completely (death). Coronary disease is the most common cardiovascular disease in the world. According to the World Health Organization (WHO), approximately 29% of deaths worldwide occurred in 2001 were due to cardiovascular disease; at least 2% are the result of coronary disease. In addition, it is estimated that coronary artery disease accounts for more than 50% of heart failure among people under 75 years old.
In the United States alone, about 16,800,000 people were diagnosed with coronary heart disease in 2006, according to American Heart Association. However, incidence varies with race and sex. In 2005, coronary heart disease death rates per 100,000 people were approximately:
- 7 for white males
- 9 for black males
- 0 for white females
- 9 for black females.
Coronary Disease Causes & Risk Factors
The occurrence of coronary disease is due to atherosclerosis, hardening of the arteries. The obstruction makes the passage of blood to the heart difficult, which leads to a deficiency of oxygen and nutrients in the heart muscle. Atherosclerosis is the result of fatty deposits (plaques) that form within the walls of blood vessels. The accumulation of these plaques reduces the diameter of the arteries, making it hard for the blood to travel to the heart.
Coronary disease is progressive medical condition that tends to develops over decades. The risk factors contributing to its development may be controllable or non controllable:
Controllable Risk Factors:
- diabetes
- Smoking
- Stress
- Physical inactivity
- obesity or overweight
- alcohol abuse
- high blood pressure (hypertension)
- cholesterol (dyslipidemia)
- radiation therapy to the chest
Non-controllable risk factors:
- Age – the risk of coronary artery disease increases with age
- gender – being male put you at higher risk of developing coronary disease
- hormonal changes – being postmenopausal
- Race – some ethnic groups such as African Americans and Mexican Americans have higher risk of coronary disease than others
- Genetics – certain genetic conditions can predispose you to atherosclerosis, which can lead to coronary heart disease.
Coronary Disease Symptoms
In early development of coronary disease, most people experience no symptoms. Symptoms begin to immerse when disease is severely damage the wall of artery. The first signs are often a chest pain called angina pectoris. The pain tends to occur during activities and disappears during rest. When the disease is severe, angina becomes unstable symptoms are less predictable and can occur even at rest. In addition, symptoms vary from individual to another and according to the severity of the disease./coronary-artery-disease-symptoms-5b4f996646e0fb00376c3e90.png)
In general, if you have coronary artery disease, you will experience at least one of these symptoms:
- Sweating
- Shortness of breath
- Fatigue and weakness
- nausea and vomiting
- burning or pressure under the clavicle
- tightness in the chest
- pain in the shoulder, jaw, arms, throat, neck or upper abdomen.
Those symptoms can also indicate a heart attack; they should not be neglected. If you experience any of them that persist for hours (not to say for days), contact your health care provider immediately. Depending on how you feel, it can be necessary to call 911.
Complications
Complications of coronary artery disease may lead to rupture of blood vessel. The rupture can completely prevent cells of the heart muscle from getting enough oxygen and nutrients they need to survive. This requires an immediate medical intervention; otherwise, heart attack or death will occur.
Heart attack symptoms are almost similar to those of coronary artery disease. Therefore, it is important to consult your doctor or call 911 if these symptoms persist. The risk of coronary disease complications or heart attack is higher if you are a smoker or have any these medical conditions:
- Obesity
- Diabetes
- High cholesterol.
Diagnosis
Your cardiologist can perform many diagnostic techniques to confirm the presence of a coronary disease in your body:
Chest X-ray – This radiographic technique allows your physician to see your rib cage in its entirety: lungs, heart, great vessels, ratings and spine. It helps him to determine the size and functioning of your heart, lungs, etc. Although a coronary disease can be suspected based on chest x-ray, additional imaging techniques are needed to accurately confirm the diagnosis.
Electrocardiogram (ECG) – This test allows your cardiologist to study the functioning of your heart by measuring its electrical activity. Each heart beat produces an electrical signal that spreads from the top of the heart to the bottom. This signal causes the heart to contract and pump blood throughout the body. Using these electrical signals, your health care provider can determine the pace of heartbeats, if the heart is dilated or overworking.
By measuring the time it takes the electrical impulse to travel through your heart, your cardiologist can determine if electrical activity is normal, fast or irregular.
Cardiac stress test – This test determines the amount of oxygen the heart receives during periods of physical activity. In addition, it can reveal any blockage of the coronary arteries. In general, a stress test is performed on a treadmill or stationary bicycle while an electrocardiograph is attached to your body. During the test, the specialist may inject a harmless radioactive substance in your blood to facilitate the study. A thallium scan is used to allow observation of blood travels during the exercise
Cardiac catheterization (heart cath) – your doctor may prescribe this exam if he suspects symptoms or signs of heart failure or malfunctioning of the heart valves. A heart cath consists of introducing a thin catheter through your blood vessel in the arm or groin into the heart chambers to measure pressure and your blood oxygen saturation level. In addition, this examination allows your cardiologist to detect reflux of blood from the aorta to the left ventricle.
Echocardiogram (cardiac ultrasound) – An echocardiogram is a medical technique consisting of using high-frequency sound waves to create picture of the heart. It is an effective technique commonly used in the diagnosis of coronary disease. A cardiac ultrasound allows your cardiologist to:
- detect heart failure
- study heart valves, mainly in search of abnormalities of the mitral valve
- Study the cardiac chambers, looking for left ventricular hypertrophy (LVH), thrombus in the left atrium, atrial dilation, etc..
CT coronary angiogram – with this recent imaging technique, your cardiologist can produce images of many part of your body. A CT coronary angiogram allows your doctor to visualize your arteries and detect fatty deposits or obstructions in the walls of your coronary arteries. CT coronary angiogram is an important tool in the coronary disease diagnosis; it provides very precise information on the functioning of the heart muscle.
Magnetic resonance angiogram (MRA) – this is a medical technique consist of using radio waves and a powerful electromagnetic field to exam blood vessels, mostly arteries of the neck thorax, abdomen, kidney and the legs. With a MRA, your cardiologist can:
- Detect the presence of an arterial aneurysm
- Detect blood vessel problems such narrowing and obstruction
- Detect an arterial plaque build-up within an arterial wall
- Check for problems in the intracranial arteries (the head), and possibly determine whether a catheter examination is required.
- Detect disease of the aorta and blood vessels that supply blood to the kidneys, brain, abdomen, lungs and legs.
Coronary Disease Treatment
 The treatment aims to facilitate the blood flow, and help the heart work better or normally. Most the time, treatment of coronary disease includes medications, coronary angioplasty or/and surgery. Depending on the severity of the artery, the treatment can be curative or palliative. During and after treatment, you should stop smoking, and regularly monitor your blood pressure and blood cholesterol. It is also important that you adopt a healthy-heart diet, manage your stress, reduce your alcohol consumption, lose weight if you are obese and practice regularly moderate exercise (approval of your doctor is needed).
The treatment aims to facilitate the blood flow, and help the heart work better or normally. Most the time, treatment of coronary disease includes medications, coronary angioplasty or/and surgery. Depending on the severity of the artery, the treatment can be curative or palliative. During and after treatment, you should stop smoking, and regularly monitor your blood pressure and blood cholesterol. It is also important that you adopt a healthy-heart diet, manage your stress, reduce your alcohol consumption, lose weight if you are obese and practice regularly moderate exercise (approval of your doctor is needed).
In general, your physician will prescribe at least one of these drugs to treat your coronary artery disease:
Cholesterol-lowering drugs – exercise and healthy eating should be the first steps against high blood cholesterol; however, they are not always effective when used without medications. If exercise and cholesterol–lowering diet do not work for you, your cardiologist will prescribe you cholesterol-lowering drugs like statins to lower your blood cholesterol to healthier levels.
Aspirin – Your doctor can recommend you to take a daily dose of aspirin or other blood thinners, along with exercise and a good diet. These substances help reduce blood clots and prevent obstruction of the coronary arteries. However, if you have bleeding disorders, aspirin is not recommended.
Beta-blockers – this class of medications is often regarded as the key drugs of cardiology; they inhibit the effects of stress on the heart, slowing heart rate and decrease blood pressure. In addition, Beta-blockers helps reduce heart oxygen needs, and prevent relapses after a heart attack.
Nitroglycerin – this medication is often used in certain heart conditions such as angina pectoris. It is available in tablets, sprays (under the tongue), continuous intravenous infusion or patch. It acts by widening the blood vessels, thereby increasing coronary blood flow and reduce blood pressure.
Calcium channel blockers – this class of medications relax the muscles in the walls of the coronary arteries, open vessels and increase blood flow around the heart, which makes the blood pressure return to normal.
Angiotensin-converting enzyme (ACE) inhibitors – Along with a heart healthy diet and exercise, ACE helps restore and maintain normal blood pressure by facilitating the pumping of blood to the heart. The ACE inhibitors may also reduce fatigue and shortness of breath, the duration of your hospitalization and thus helps you live longer with the disease. In fact, studies have shown that these drugs may reduce the risk of heart attack, stroke and death in people with a history of coronary disease.
Coronary Disease Prevention
Changes in lifestyle, taking drugs and surgical intervention can treat coronary artery disease. However, in spite of precaution, the disease can cause death. In fact, coronary heart disease remains a leading cause of death worldwide. Therefore, if you are at risk of coronary disease, it is important that you check your cardiovascular system regularly to prevent sudden death.
An electrocardiogram (EKG) can detect early abnormalities of the heart’s electrical charges, and initiate appropriate treatment before the problem becomes more complicated. Even if you’re not at risk, it is important to:
- not smoke
- exercise regularly
- not abuse alcohol
- prevent or/and control high blood pressure and high cholesterol
- treat your diabetes, if you are diabetic
- lose or maintain a healthy weight
- reduce stress in your life
- eat healthy foods, in avoiding sugar, white flower, saturated fat and all products containing it.
References:
1 – The World Health Report 2002: Reducing risks, promoting healthy life
2 – Le diagnostic de la maladie coronarienne : Brochure d’information à l’ intention du patient offerte par la Fondation Suisse de Cardiologie
3 – http://www.americanheart.org/presenter.jhtml?identifier=4576
4 – Kontos, MC; Diercks, DB; Kirk, JD (Mar 2010). “Emergency department and office-based evaluation of patients with chest pain”. Mayo Clinic Proceedings 85 (3): 284–99. doi:10.4065/mcp.2009.0560. PMID 2019415
5 – Kivimäki M, Nyberg ST, Batty GD, Fransson EI, Heikkilä K, Alfredsson L, Bjorner JB, Borritz M, Burr H, Casini A, Clays E, De Bacquer D, Dragano N, Ferrie JE, Geuskens GA, Goldberg M, Hamer M, Hooftman WE, Houtman IL, Joensuu M, Jokela M, Kittel F, Knutsson A, Koskenvuo M, Koskinen A, Kouvonen A, Kumari M, Madsen IE, Marmot MG, Nielsen ML, Nordin M, Oksanen T, Pentti J, Rugulies R, Salo P, Siegrist J, Singh-Manoux A, Suominen SB, Väänänen A, Vahtera J, Virtanen M, Westerholm PJ, Westerlund H, Zins M, Steptoe A, Theorell T (October 2012). “Job strain as a risk factor for coronary heart disease: a collaborative meta-analysis of individual participant data”. Lancet 380 (9852): 1491–97. doi:10.1016/S0140-6736(12)60994-5. PMC 3486012. PMID 22981903.
6 – Lee IM, Shiroma EJ, Lobelo F, Puska P, Blair SN, Katzmarzyk PT (July 2012). “Effect of physical inactivity on major non-communicable diseases worldwide: an analysis of burden of disease and life expectancy”. Lancet 380 (9838): 219–29. doi:10.1016/S0140-6736(12)61031-9. PMC 3645500. PMID 22818936.
7- “Agent Orange: Diseases Associated with Agent Orange Exposure”. Department of Veterans Affairs Office of Public Health and Environmental Hazards. 25 March 2010. Archived from the original on 9 May 2010. Retrieved 5 May 2016
8 – Wang HX, Leineweber C, Kirkeeide R, Svane B, Schenck-Gustafsson K, Theorell T, Orth-Gomér K (March 2007). “Psychosocial stress and atherosclerosis: family and work stress accelerate progression of coronary disease in women. The Stockholm Female Coronary Angiography Study”. J. Intern. Med. 261 (3): 245–54. doi:10.1111/j.1365-2796.2006.01759.x. PMID 17305647
9 – Underwood and Cross, James (2009). General and Systematic Pathology. London, UK: Churchhill livingstone. p. 279.
10 – Kannel, WB; Vasan, RS (Jul 2009). “Triglycerides as vascular risk factors: new epidemiologic insights.”. Current opinion in cardiology 24 (4): 345–50. doi:10.1097/HCO.0b013e32832c1284. PMC 3012388. PMID 19424059.
11 – Danesh J, Collins R, Peto R (2000). “Lipoprotein(a) and coronary heart disease. Meta-analysis of prospective studies”. Circulation 102 (10): 1082–85. doi:10.1161/01.CIR.102.10.1082. PMID 10973834.
12 – Smolders B, Lemmens R, Thijs V (2007). “Lipoprotein (a) and stroke: a meta-analysis of observational studies”. Stroke 38 (6): 1959–66. doi:10.1161/STROKEAHA.106.480657. PMID 17478739.
13 – Schreiner PJ, Morrisett JD, Sharrett AR, Patsch W, Tyroler HA, Wu K, Heiss G (1993). “Lipoprotein(a) as a risk factor for preclinical atherosclerosis” (PDF). Arterioscler. Thromb. 13 (6): 826–33. doi:10.1161/01.ATV.13.6.826. PMID 8499402.
14 – “Scientific Report of the 2015 Dietary Guidelines Advisory COmmittee” (PDF). health.gov. Feb 2015. p. Part D, Chapter 1, Page 17 (642