Table of Contents
Gingiva, (gums) is a part of the oral mucosa, the soft membrane lining of the mouth. It surrounds the root of each tooth and covers the alveolar bone. As the teeth, the gingiva contains keratin (a family of scleroproteins) that makes it strong and resistant. A healthy gum is usually coral pink and non- hemorrhagic. However, your gingiva can be affected by infection, which makes it bleeds, swells or changes color. When that happens, you have a type of gum disease (periodontal disease) called gingivitis.

Gingivitis is the inflammation of your gums due to an overgrowth of bacteria on your oral mucosa, precisely between your teeth and gums. Those bacteria are naturally found in your mouth, they are not pathogenic. Under certain circumstances, they overgrow and cause periodontal diseases. Gingivitis begins with formation of plaque, a sticky and transparent film of bacteria that forms on your teeth every day. If these microorganisms are not removed regularly, they will eventually harden and turn into tartar, a yellow or brown color mineral build up that only a dental professional can remove.
Gingivitis Causes
Although many factors are susceptible to the development of gingivitis, bacteria remain the major cause. When there is poor or lack of oral hygiene (brushing and flossing), certain bacteria such as Streptococcus mutans and anaerobes seep into the bone at the root of your teeth and build up a thick layer. This layer is made of bacteria, mucus and thin particles of food, mostly starches and sugars. Those bacteria hide at the base of your gums (gumline). If they are not removed in about 3 days, they form a hard colored layer called tartar. Unlike gingivitis and some other periodontal infections, tartar is more serious and required special care of dentist.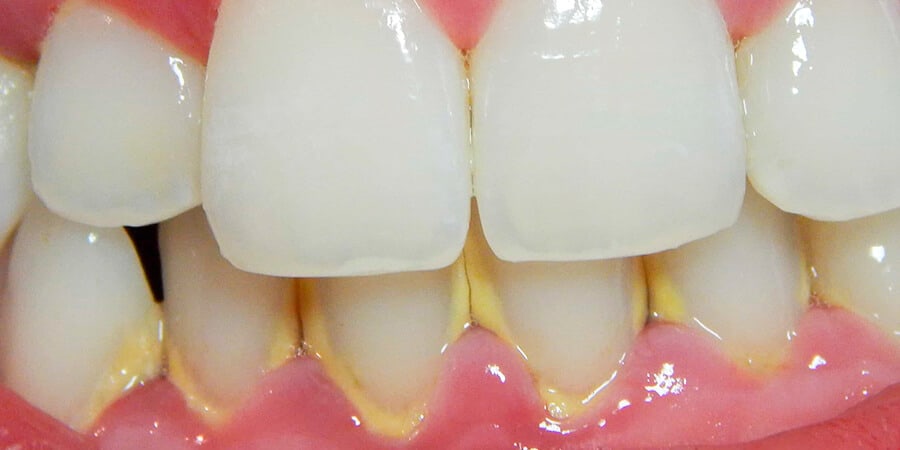
Gingival bleeding is another cause of ginvitis. When the gum bleeds, it tends to become swollen, a favorable factor for overgrowth of Streptococcus mutans and anaerobes.
Poor oral hygiene can also lead to gingitis, tatar, and other serious disease such as cardio vascular disease. In women, temporary hormonal changes can also cause gingivitis. Although rare, some antidepressants or antiepileptic drugs are also potential causes of gingivitis.
Gingivostomatitis herpetic – Sometimes, gingivitis can be caused by viral infection. Viruses most likely to affect your gums are the herpes simplex virus 1 and 2 (HSV-1 and HSV-2). Those pathogenic microorganisms create tiny perforations and ulcers in the gums and other parts of your mouth. This can lead to extensive gangrenous plaque resulting in infection and bleeding; this medical condition is called gingivostomatitis herpetic or ulceronecrotic gingivitis.
Ulceronecrotic gingivitis –this medical condition is the result of rapid destruction of the gums and the alveolar bone. It occurs mostly in adolescents and in patients suffering from immune deficiency. If left untreated, the disease can evolve rapidly towards ginvitis and other periodontal problems.
Risks of gingitis – Some people are more likely to have gingivitis. Gingivitis affects particularly immunocompromised individual such as people with diabetes, AIDS, or leukemia. Other factors increasing the risk of gingivitis include:
- Stress
- Puberty
- Pregnancy
- Menopause
- Cancer and its treatment
- Loose dentures
- Cigarette smoke
- Misaligned teeth
- Vitamin C deficiency
- Vitamin B3 (niacin) deficiency
- Use of certain contraceptive pills
Gingivitis Symptoms
Like dental cavities, early-stage of gingivitis is painless, which could make you have the disease without being aware of it. When signs and symptoms finally occur, they may include:
- Mouth sores
- Foul breath (Halitosis)
- Soft and swollen gums
- Bad taste
- Shiny appearance to gums
- Bleeding gums (mostly during brushing of the teeth)
- Gum discoloration (bright red or red-purple)
Gingivitis Diagnosis
Gingivitis diagnosis is based primarily on the appearance of your gums. Absence of a coral pink color of the gum is already a sign indicating to your dentist there is something wrong. After that superficial exam, the dentist will take a closer look to examine your mouth and teeth to look for gingivitis signs, mouth sores, soft, or red-purple gums. Once gingivitis signs are found, you dentist will examine the inflammation, which can help her/him to distinguish bacterial infection of a herpes virus.
In rare cases, mostly when there are complications, your dentist may recommend dental x-rays and biopsies to get more information on the species of the bacteria infecting your gum. Biopsy is also recommended to rule out other diseases such as diabetes or leukemia.
Gingivitis Treatment
The first step in treating gingivitis is to reduce the inflammation by removing all those harmful microorganisms causing plaque and tartar. One of two common methods your doctor can choose to get rid of those etiologic agents are Scaling or root planning, non-surgical periodontal therapies used to clean plaque and tartar from your teeth. If you have bleeding gums, the cleaning may be a little painful or uncomfortable, but the pain is usually minor.
After the deep cleansing, regular brushing and flossing is necessary to prevent reoccurrence of the infection. In addition, misaligned teeth or dental and orthodontic appliances should be repaired or replaced if they were the causes of the gingivitis.
Gingivitis Prevention
Regular use of dental floss and anti tartar toothpaste can prevent not only gingivitis and tartar, but also many other oral diseases. Here are some tips that can help you prevent gingivitis and maintain a good oral health:
- Check your gums regularly, and look for signs of gingivitis and dental problems
- Report immediately to your dentist symptoms of sensitive teeth or bleeding gums
- Eat a healthy diet rich in vitamin C and vitamin B3 (niacin)
- Brush your teeth and your tongue twice a day or after each meal
- Use dental floss once a day to remove plaque between your teeth
- Avoid too much sugar in your diet; it is a major cause of dental problems
- Do not smoke; cigarette smoke is one of the leading factors of developing dental problems and oral cancer
- See your dentist regularly for exams and get your teeth cleaned, and stains or tartar removed.



