Table of Contents
Mitral Valve Prolapse
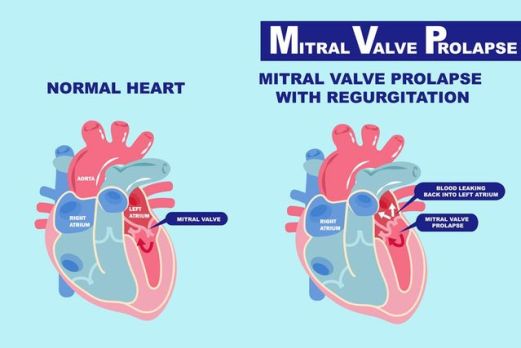
The mitral valve separates the left atrium from the left ventricle. During ventricular diastole, it opens to allow passage of blood flow from the left atrium to left ventricle. While during ventricular systole, it closes to keep blood from backflowing from the ventricle to the atrium.
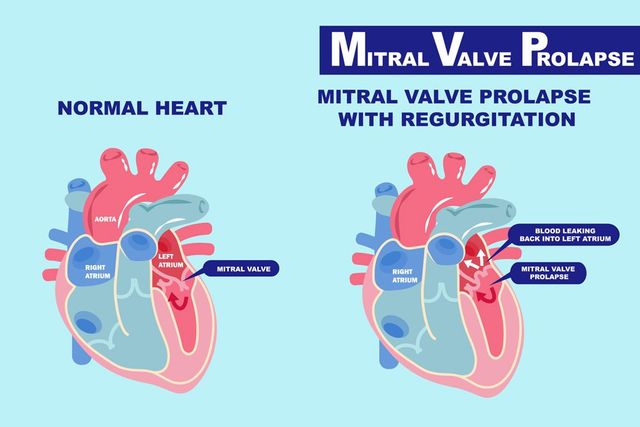 Mitral valve prolapse, also known as floppy mitral valve, Barlow’s syndrome or murmur syndrome, is a disorder of functioning of the mitral valve characterized by incomplete closure of the mitral valve orifice. The condition makes the blood flows back from the ventricle to the atrium during contraction of the ventricles (ventricular systole).
Mitral valve prolapse, also known as floppy mitral valve, Barlow’s syndrome or murmur syndrome, is a disorder of functioning of the mitral valve characterized by incomplete closure of the mitral valve orifice. The condition makes the blood flows back from the ventricle to the atrium during contraction of the ventricles (ventricular systole).
Unlike many other heart diseases, mitral valve prolapse it is often asymptomatic. Some patients may live years with the disease without experiencing any disturbing symptoms. Most of the times, mitral valve prolapse is not life-threatening. However, if left untreated, a mitral valve prolapse can lead to arrhythmic complications, which require immediate medical attention.
Incidence
Mitral valve prolapse is a very frequent cardiac disorder. It is estimated that 2-3% of the world population is affected by the disorder, according to the Framingham Heart Study, a cardiovascular study led by Dr. Lisa A. Freed, in Framingham, Massachusetts. Contrary to what most scientists believed, the new study has shown that mitral valve prolapse has no predominance among women; both men and women are equally affected by the disease.
Causes and Risk Factors
The role of the mitral valve is to control the blood flow from the atrium (one of the two upper chambers of the heart) to the left ventricle of the heart. When the mitral valve is healthy, the blood flows in one direction, from the top (atria) to the bottom chambers of the heart (ventricles). When the mitral valve prolapses, instead of one-way, blood flows back into the atrium.
In most cases, the cause of mitral valve prolapse is not well known. However, genetic disorders are suspected to be linked to the development of the disease:
- Ebstein’s anomaly (also known as Ebstein’s malformation – a congenital heart defect)
- Marfan syndrome – a disorder characterized by functioning of the connective tissue
- Adult polycystic kidney disease –presence of one or multiple cysts in one or both kidneys
- Scoliosis – an abnormal curvature of the spine
- Ehlers-Danlos syndrome – a group of connective tissue disorders characterized by extremely loose joints, hyperelastic skin that bruises easily, and easily damaged blood vessels.
In addition, theses following medical conditions can contribute to the development of mitral valve prolapse:
- previous heart attack
- rheumatic fever
- graves’s disease (Basedow’s disease)
- ischemic heart disease– reduced blood supply to the heart muscle
- endocarditis Osler – occurrence of painful and red lesions on the palms and soles
- atrial septal defect – a form of congenital heart defect characterized by a hole in the heart, precisely between the two atria.
Warning Signs and Symptoms
You can live with mitral valve prolapse for years without experiencing any symptoms. In fact, the majority of patients learn they have the disease during a diagnosis for another medical condition. When symptoms finally emerge, they develop gradually and tend to vary from one person to another. Usually, if you have a symptomatic mitral valve prolapse, you will experience at least one of the following symptoms:
- anxiety
- dizziness
- palpitations
- shortness of breath
- lightheadedness
- unreasonable fatigue
- irregular heartbeat (arrhythmia)
- shortness of breath, mostly during physical activity
- chest pain that is not related to coronary artery disease or heart attack.
Complications
Although rare, sometimes mitral prolapse may be accompanied with the following complications:
- blockage (occlusion) of blood vessel
- mitral valve regurgitation
- heart valve infection (endocarditis)
- abnormal rhythm problems (arrhythmias).
Diagnosis
First thing your cardiologist will do is a physical exam. During the physical examination, your doctor will examine your heart functioning with a stethoscope. Generally, mitral valve prolapse produces a specific heart murmur that allows your cardiologist to identify the disease. However, other medical examinations will be performed to confirm the diagnosis. Those tests allow your physician to visualize blood flow, and accurately confirm the diagnosis.
Echocardiogram – this painless exam consist of using sound waves to create picture of your heart muscle. It allows your cardiologist to view your heart in motion on a screen. The images show if your heart muscle is working well or not. Echocardiogram also provides anatomic information of your heart such as size and shape.
Coronary catheterization (angiogram) – this diagnostic and therapeutic technique consists of using a thing catheter along with a computerized tomography to examine the circulation of blood in the vessels of the heart muscle. Using the procedure, your cardiologist can detect not only how blood circulate in your heart but also measure the blood pressure and oxygen levels. The angiogram can also detect narrowing or blockage in the coronary arteries. In addition, a coronary catheterization can be used to detect narrowing or blockage of the carotid arteries, vessels that bring blood from the heart to the brain.
Chest X-ray – this exam allows your doctor to evaluate organs in your thoracic cage such as lungs, heart and chest wall. A chest X-ray not only helps visualize the size and shape of your heart, but also helps discover major cardiac pathologies such as heart failure and other diseases of the heart muscle.
Nuclear Heart Scan – this cardiac exam allows your cardiologist to evaluate the health of your heart. During the procedure, a radioactive material called tracer is used to examine your left and right ventricular functions. Usually, left ventricular function is impaired in individual with mitral valve prolapse; your doctor will recommend this test to see if your heart normally pumps blood through different parts of your heart muscles.
Cardiac stress test – also called exercise stress test, cardiac stress test is an examination done by a cardiologist as a part of heart disease diagnosis. During the test, your cardiovascular system submitted to a short and intense effort, which allows your physician to measure your heart rate and detect cardiovascular problems: abnormal blood flow to your heart, high blood pressure, shortness of breath, etc. having those details, your doctor is able to recommend you an appropriate treatment or other more specialized exams: coronary angiography, myocardial scintigraphy, etc.
Electrocardiogram (ECG) – ECG is a graphic representation of the electric potential that controls the activity of your heart muscle. This painless test can be done in your doctor’s office, hospital or at home. However, its interpretation remains complex; it requires the help of a health care professional.
Mitral Valve Prolapse Treatment
In most cases, no treatment is necessary. Your doctor will recommend you to practice some preventive measures to stop the progression or evolution of the disease, which may include but not limited to:
- adoption of a heart healthy diet
- avoidance of cardiac stimulants: caffeine, alcohol, etc..,
- avoidance of all medications that accelerate the heart concentration,
- doing moderate physical exercise regularly.
Although it is not recommended by American Heart Association, some cardiologists, however, recommend their valve mitral prolapse patients to take antibiotics before dental or surgical operations to prevent endocarditis, an inflammation of the membrane that lines the inner heart.
In case the disease produces severe symptoms such as chest pain, anxiety, panic attacks, treatments are needed. Mitral valve prolapse treatment can be drug therapy, surgical therapy or both.
Medications
Aspirin – Aspirin acts on the platelets by inhibiting cyclooxygenase (COX), an enzyme that plays an important role in making the platelets clump together and cause blood clotting (platelet aggregation). A daily dose of aspirin can promote blood circulation and prevent formation of blood clots.
Beta blockers – Beta blockers are drugs used to treat certain heart problems such as angina attacks. In addition, they can be used to prevent excessive cardiac stress and stabilize blood pressure. Besides mitral valve prolapse and angina, beta blockers are used to treat the following cardiac conditions:
- heart attack
- hypertension
- heart Failure
- cardiac arrhythmias (abnormal rate/rhythm of the heartbeat)
- hyperthyroidism (overproduction of thyroid hormone by the thyroid gland)
- panic disorder (formerly called cardiac neurosis)
- Hypertrophic cardiomyopathy (thickness of the heart muscle).
Anticoagulants – this class of drugs helps prevent formation and growth of blood clots, reduce the risk of heart attack, stroke (stroke) and blockage of arteries and veins. Anticoagulants are often used to treat patients with artificial heart valve or those who suffer from any of the following conditions:
- heart attack
- stroke
- cardiomyopathy
- Any disease that increases the risk of blood clots formation.
Surgical therapy
Surgery is not always necessary in the treatment of mitral valve prolapse. In some cases, however, leakage of blood can become serious and requires an operation of the mitral valve. In this case, your cardio surgeon will perform a surgery to repair or replace the diseased mitral valve with an artificial or healthy biological one.
Mitral valve repair – In case the valve diseased is not too damaged to be repaired, your cardio-surgeon may perform a mitral valve repair. This surgical procedure consists of removing excess valve tissue, tightening or replacing the valve annulus – the ring of tissue supporting the valve.
Unlike the valve replacement, this method allows your health care provider to preserve your own valve, thus preventing implantation of prosthesis and taking of anticoagulant drugs. In fact, this method is the best option for most patients with non advanced mitral valve prolapse. Mitral valve repair ensure a better long-term survival and a faster recovery than the valve replacement. In addition, the repair presents a lower risk of stroke and endocarditis.
Heart valve replacement – the replacement of the diseased valve is performed when all other alternatives fails to produce satisfying results. The goal of the replacement is to improve or eliminate symptoms and reduce the risk of impact on the function of the heart. The operation must be performed in a cardiac surgery center after completion of a preoperative evaluation indicates that there is no contraindication for the intervention.
Mitral Valve Prolapse Prevention
There is no known method to prevent mitral valve prolapse. Once you have the disease, the only option is to take preventive steps indicated by your physician to prevent development of complications associated with it. However, to reduce your risk of having all cardiovascular diseases, you need to:
- excise regularly
- lose weight (if you are obese or overweight)
- Stop smoking (including second hand smoke).
In addition, you need to avoid fast foods and adopt a healthy diet.
- Increase your intake of antioxidants
- Avoid saturated acids, mainly from animal fats, pastries, margarine, etc.
- Increase your intake of carbohydrates and fiber; they play an important role in increasing the levels of good cholesterol
- Reduce bad cholesterol in your diet: egg yolk, organ meats (brain, kidney, liver), nuts, almonds, lobster, shellfish, fish eggs, etc.
- Eat regularly unsaturated fatty acids such as omega-6 (sunflower oil) omega 3 (flax seed oil, fish oil), they lower the bad LDL cholesterol and prevent the formation of a blood clot.
- Eat plenty fruits (2 to 3 per day), vegetables (3 to 4 servings per day), polyphenols (moderate consumption of wine and green tea) and phyto-oestrogens: soy, green tea, chickpeas, lentils, beans, grains, carrots, fennel, onions, garlic, etc.
1- J. Quevauvilliers, L. Perlemuter, Le dictionnaire médical de l’infirmière, Editions Masson, Paris.
2 – Univ. of Pittsburgh Medial Center (UMPC), Mitral valve prolapse, novembre 2006 (page consultée le 17 décembre 2007
3 – Doctissimo.com, Encyclopedia medicale, L’insuffisance mitrale
4 – http://www.framinghamheartstudy.org/biblio/2002.html
5 – http://www.nlm.nih.gov/medlineplus/ency/article/001468.htm
6 – “Related Disorders: Mitral Valve Prolapse”. Archived from the original on 2007-02-25. Retrieved 2007-07-11.
7- Lumiaho, A; Ikäheimo, R; Miettinen, R; Niemitukia, L; Laitinen, T; Rantala, A; Lampainen, E; Laakso, M; Hartikainen, J (2001). “Mitral valve prolapse and mitral regurgitation are common in patients with polycystic kidney disease type 1”. American Journal of Kidney Diseases 38 (6): 1208–16. doi:10.1053/ajkd.2001.29216. PMID 11728952.
8 – “Mitral Valve Prolapse Overview”.
9 – “Pectus Excavatum: Epidemiology”. Medscape. Retrieved 14 April 2016.
10 – Playford, David; Weyman, Arthur (2001). “Mitral valve prolapse: time for a fresh look”. Reviews in Cardiovascular Medicine 2 (2): 73–81. PMID 12439384.
11 – Freed LA, Levy D, Levine RA, Larson MG, Evans JC, Fuller DL, Lehman B, Benjamin EJ. (1999). “Prevalence and clinical outcome of mitral-valve prolapse”. N Engl J Med 341 (1): 1–7. doi:10.1056/NEJM199907013410101. PMID 10387935.
12 – Cotran, Ramzi S.; Kumar, Vinay; Fausto, Nelson; Nelso Fausto; Robbins, Stanley L.; Abbas, Abul K. (2005). Robbins and Cotran pathologic basis of disease. St. Louis, Mo: Elsevier Saunders. ISBN 0-7216-0187-1.
13 – NLM/NIH: Medline Plus Medical Encyclopedia: Rheumatic fever
14 – S Venkatesan; et al. (Sep–Oct 2007). “Can we diagnose Infective endocarditis without vegetation?”. Indian Heart Journal 59 (5).
15 – Mitral Valve Prolapse at eMedicine
16 – Rodgers, Ellie (May 11, 2004). “Mitral Valve Reg