Table of Contents
Osteomyelitis, commonly called bone infection, is a degenerative infection affecting your bone or bone marrow. It is the result of bacteria (pyogenic bacteria or mycobacteria) and rarely fungus. Osteomyelitis is a serious medical condition that often affects the long bones in children, and the vertebrae and pelvis in adults. Without a proper treatment, the disease gradually destroys the bones and damages the joints, causing serious physical disabilities or death of the bone tissue.
Osteomyelitis may be acute or chronic:
Acute Osteomyelitis – is a type of infection occurring mostly in children. It presents as a pus-producing infection accompanied by edema, vascular congestion, and small-vessel thrombosis (formation of a blood clot inside small blood vessels)
There are two primary categories of acute Osteomyelitis:
- Hematogenous osteomyelitis is a form of Osteomyelitis affecting primary children and accounts for almost 20% of cases of osteomyelitis. Bacteria causing the Infection coming from a remote site, and usually affects a single bone.
- Direct or Contiguous inoculation osteomyelitis – occurs where there is direct contact of infected tissues with bone which may occur during a surgical procedure or following trauma. Clinical manifestations of direct inoculation osteomyelitis are more localized than those of hematogenous osteomyelitis and there are often multiple organisms involved.

Chronic Osteomyelitis – is a severe, persistent, and sometimes incapacitating infection of bone and bone marrow. It is often a recurring condition because it is difficult to treat definitively. This disease may result from:
- Inadequately treated acute osteomyelitis
- Hematogenous type of osteomyelitis
- Trauma
- Iatrogenic causes such as joint replacements and the internal fixation of fractures
- Compound fractures
- Infection with organisms, such as Mycobacterium tuberculosis and Treponema species (syphilis)
- Contiguous spread from soft tissues, as in diabetic ulcers or ulcers in peripheral vascular disease (eMedicine source).
Osteomyelitis Causes
Osteomyelitis is always caused by either a pathogenic bacterium or by fungus. The bacterium that is mostly triggering the infection is Staphylococcus aureus.
Human bones are generally well protected and do not become infected easily. Unlike certain organs in our body, the bones are not exposed directly to aggressors. For an infection to occur, it requires at least three factors:
- Fracture – pathogenic microorganisms enter the bone due to a fracture
- Infectious organisms in Soft tissue – infection that have been present in soft tissue spreading to the bones via the bloodstream
- Infectious organisms in the blood – infection that have been present in the blood contaminating the bones
Other Risk factors may include Disease and Lifestyle:
- peripheral vascular disease
- chronic swelling
- poor circulation
- diabetes
- weaken immune system
- severe wound
- cigarette smoking
- poor diet
- Malnutrition
- Poor hygiene
- Walking barefoot on a hard ground, etc.
Osteomyelitis Symptoms
 The symptoms of osteomyelitis start by an intense pain in the bone accompanied with local swelling, redness, and warmth. Children may complain of high fever, nausea and malaise (general feeling of discomfort or uneasiness).
The symptoms of osteomyelitis start by an intense pain in the bone accompanied with local swelling, redness, and warmth. Children may complain of high fever, nausea and malaise (general feeling of discomfort or uneasiness).
Adults may not have fever, but the symptoms swelling, redness and pain are progressive and more severe. They may also suffer from Low back pain and Swelling of the ankles, feet, and legs
Osteomyelitis Diagnosis
Usually, to diagnose the disease, the doctor would do physical examination to search for swelling, redness and bone tenderness. Your physician may take sample of blood (Blood cultures), pus, fluid (needle aspiration biopsy) and articular bone tissue (bone lesion biopsy) for analysis purposes. The doctor may do a cerebrospinal fluid (CSF) specimen collection with a needle or at by orthopaedic surgery.
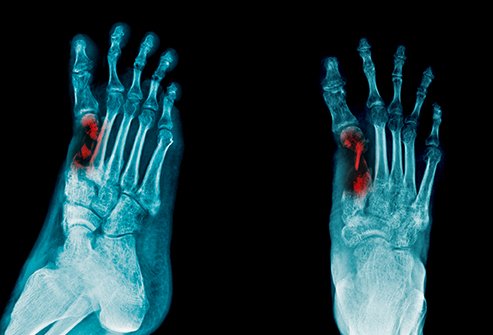
In most cases, X-ray is associated with the tests. Types of X-ray may include bone x-ray, joint x-ray, hand x-ray, extremity x-ray, etc.
Osteomyelitis Treatment
The type of treatment you are given depends on the severity of the infection, the organ affected and the cause of the disease. However, in any circumstance, osteomyelitis requires an immediate treatment. The treatment may consist of antibiotherapy along with immobilization of the bone infected with a plaster; or surgery, removal and transplantation of bone.
If the disease is caused by blood-borne infection, (infectious agents that are spread by blood) high doses of antibiotics treatment can be used. Your doctor would prescribe antibiotics (Clindamycin, Levaquin, Amoxicillin, Bactrim, etc.) that are capable to destroy the bacteria causing the infection.
If the infection is the cause of a foreign body in the organism (prosthesis), surgical intervention is necessary to remove the prosthesis and to replace it. In general, antibiotics are administered before and after the surgery. In case antibiotherapy and surgery do not bring good result (mostly in diabetic people), the surgeon will have to amputate the infected organ.