Table of Contents
Pneumonia is a lung infection caused by bacteria (bacterial pneumonia), viruses (viral pneumonia), fungus, parasite, rarely chemical or physical irritant agents. The disease results in an alveolitis, inflammation of the alveoli (tiny air sacs within your lungs).
When you have pneumonia, your alveoli are filled with secretions and become unable to effectively distribute oxygen in your blood. There are effective pneumonia treatments; however, depending on the type of infectious agents causing the infection, hospitalization or even death can occur. Those complications happen, most of the times, among the elderly and individuals suffering from chronic obstructive pulmonary diseases (COPD) or HIV / AIDS. Although pneumonia can affect any group of people, it is more common among young children, elderly, and immunocompromised individuals:
- Cancer patients
- AIDS/ HIV patients
- Hemodialysis patients
- Organ transplant recipients
- Malnourished people
- Those who do not get enough sleep
- Patients receiving immunosuppressive drugs.
Pneumonia Incidence
Pneumonia is very common in the world. According to a study done by researchers at the Boston University School of Public Health with support from the World Health Organization (WHO) and the U.S.  Agency for International Development (USAID), Pneumonia is the leading cause of mortality in the world among children under five; it is responsible for the deaths of nearly four children every minute. In the United States alone, each year, more than 3 million people are diagnosed with pneumonia, killing at least 5% of them.
Agency for International Development (USAID), Pneumonia is the leading cause of mortality in the world among children under five; it is responsible for the deaths of nearly four children every minute. In the United States alone, each year, more than 3 million people are diagnosed with pneumonia, killing at least 5% of them.
Pneumonia Causes and Risk Factors
Depending on its causes, pneumonia is grouped in different types:
Community-acquired pneumonia (CAP) – you acquire this type of pneumonia during your routine activities without having recently been hospitalized. CAP is commonly caused by Streptococcus pneumoniae (also called pneumococcus, a pathogenic bacterium commonly found in the nose and throat) and sometimes mycoplasma pneumoniae (a small bacterium that does not contain a cell wall). Community-acquired pneumonia is often characterized by cough, fever, chills, fatigue, dyspnea, rigors, and chest pain.
The following are some of the common factors that increase your risk of contracting community-acquired pneumonia:
- Alcohol abuse
- Being 65 or older
- Being Native American
- Smoking, including second hand smoke
- Prolonged exposure to certain chemicals, air pollution or toxic fumes
- Having one or more of the following chronic illnesses: HIV/AIDS, diabetes, cancer, cardiovascular disease, lung diseases such as emphysema.
Hospital-acquired pneumonia (HAP) – also called nosocomial pneumonia, HAP is an infection contracted during a hospital stay at least 48 hours after you were admitted. This type of pneumonia tends to be associated with higher rates of morbidity than community acquired pneumonia. Approximately 2% of nosocomial pneumonia has major complications; HAP is responsible for a prolongation of hospital stay of 7 days on average, and associated with an overall mortality of 20 to 40% of cases.
Some major risk factors for Hospital-acquired pneumonia include:
- Stroke
- Being elderly
- Major surgery
- Cardio-pulmonary disease
- Malnutrition
- Co-morbidities (coexisting medical conditions in addition to a primary disease)
- Being previously diagnosed/treated with Pneumonia
- Taking inhaled corticosteroids for more than 24 weeks
- Receiving prolonged intensive care in hospital
- Being fed by nasogastric tube
- Being treated with immunosuppressive drugs or immunosuppressive agents
- Taking antacids/And-H2
- Receiving PEEP (positive end-expiratory pressure).
Aspiration pneumonia – also called anaerobic pneumonia or bronchial pneumonia, aspiration pneumonia is occurs when chemical substances enter the bronchial tubes and cause inflammation of the lungs and the airways of the lungs. In addition, aspiration pneumonia can be caused by accidental aspiration of food, vomiting or stomach acid into the lungs. Substance sucked up in the lungs can also lead to inflammation of the alveoli (alveolitis).
Although rare, strokes, Parkinson’s disease, amyotrophic lateral sclerosis (ALS) can also contribute to the development of aspiration pneumonia.
Viral pneumonia – viral pneumonia refers to inflammation of the lungs due to the presence of viruses in the bronchial tree, mostly the influenza virus, respiratory syncytial virus (RSV), herpes simplex virus (HSV), parainfluenza virus, adenoviruses or metapneumovirus (hMPV). Herpes simplex virus (HSV) rarely causes pneumonia; when it occurs, it is mostly in infants. There is also a high risk of viral pneumonia in immunosuppressed people due to overgrowth of cytomegalovirus (CMV).
Bacterial pneumonia – the air you breathe is full with bacteria in suspension. These microorganisms can remain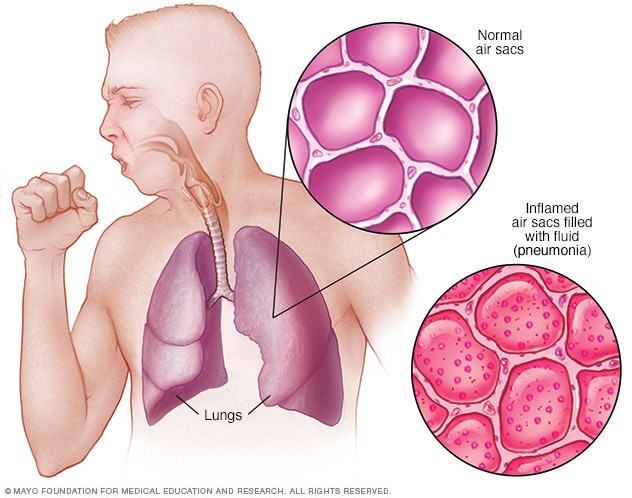 in your upper respiratory tract (such as nose, mouth and sinuses) or enter your lungs and the alveoli. Once in the alveoli, those pathogenic microorganisms invade the spaces between cells and alveoli and penetrate the bloodstream causing serious health problems including pneumonia.
in your upper respiratory tract (such as nose, mouth and sinuses) or enter your lungs and the alveoli. Once in the alveoli, those pathogenic microorganisms invade the spaces between cells and alveoli and penetrate the bloodstream causing serious health problems including pneumonia.
This bacterial invasion causes the immune system to produce a group of white blood cells called neutrophil granulocytes (or neutrophils) as a mechanism of defense; this is done to protect the body. If the immune system is strong, it will successfully fight the bacterial attack; if it is too weak, the bacteria will overcome and cause diseases such as pneumonia. That is, you are at higher risk of having bacterial peneumonia if your immune system is waek, which can be due to:
- Organ transplant
- HIV/AIDS
- Taking immunosuppressive drugs
- Having heart defects
- Being elderly
- Having a chronic disease
Fungal pneumonia – Fungal pneumonia is a rare form of pneumonia developed in people with weakened immune system due to certain factors such as AIDS, immunosuppressive drugs, or certain types of cancer. Common fungi that are responsible for this infection include:
- Histoplasma capsulatum
- Cryptococcus neoformans
- Blastomyces
- Pneumocystis jiroveci
- Coccidioides immitis.
Other forms of transmission – Some forms of pneumonia can be caused by the same viruses that cause colds and flu (parainfluenza virus for instance). They are transmitted by contact of hands or by tiny droplets released in the air through mouth and nose when pneumonic people laugh, sneeze or cough. The disease caused by these viruses depends on the organ affected: when the pathogen affects the upper respiratory tract, you will tend to have a cold; if they affect the lungs, you can develop pneumonia.
Pneumonia Signs and Symptoms
Pneumonia symptoms tend to vary depending on the causative agent or the health of the victim. Usually, pneumonia symptoms are more severe among elderly and people with compromised health.
Common symptoms of pneumonia are mostly:
- Fever
- Shaking chills
- Rapid, shallow breathing or chest breathing
- Shortness of breath
- Sharp or stabbing chest pain worsened by deep breathing or coughing
- Cough associated with greenish or yellow mucus, and occasional bloody sputum.
Some people may also experience the following symptoms:
- Headache
- Excessive sweating
- Clammy skin (lack of normal skin color)
- Loss of appetite
- Excessive fatigue
- Confusion, especially in older people.
Pneumonia Diagnosis
 Usually, pneumonia diagnosis begins with a physical examination of your lungs. Your physician will listen to your lungs and search your medical history. These steps, however, are not sufficient to confirm the diagnosis; it is confirmed by chest x-ray and blood and mucus tests.
Usually, pneumonia diagnosis begins with a physical examination of your lungs. Your physician will listen to your lungs and search your medical history. These steps, however, are not sufficient to confirm the diagnosis; it is confirmed by chest x-ray and blood and mucus tests.
Chest x-ray – this radiographic exam helps your doctor detect in your lungs anomalies such as a white area or a lung segment, which can explain the presence of pneumonia. The chest x-ray also allows your health care provider to determine the location and extension of the inflammation.
Blood tests – mucus and blood tests are done to measure your white blood cells count (WBC, Leukocyte count) and detect microorganisms in your blood. The white Blood Cell Count test is also important to rule out other medical conditions having symptoms similar to pneumonia: respiratory infection, allergy, leukemia, etc.
Mucus test – your doctor can recommend a mucus test to look for microorganisms in your lung secretion.
Pneumonia Treatment
The treatment of pneumonia depends on your age, your health, results of the exams and where the pneumonia was contracted: community-acquired pneumonia or hospital-acquired pneumonia. For instance, treatment of a pneumonia contracted in hospital is always more intense; viral pneumonia does not require the same treatment as bacterial pneumonia:
Bacterial pneumonia – if you have a bacterial pneumonia, the treatment involves the use of antibiotics (to kill the germs) associated with analgesics (pain killers) to relieve chest pain and reduce fever. Most of the times, your doctor will recommend you to take ibuprofen or paracetamol. It is very important to follow the treatment completely and as prescribed to avoid relapsing of the infection or a serious form of pneumonia called drug-resistant pneumonia. In some more severe cases, antibiotics may be associated with hospitalization to:
- Put you on oxygen
- Administer the antibiotics intravenously
- Moisturize your body by injecting fluids intravenously.
Viral pneumonia – viral pneumonia are often less severe than bacterial pneumonia, in most cases, the infection goes on its own in less than three weeks without treatment. Some severe infection, however, may be required medical treatment. However, unlike the treatment of bacterial pneumonia, antibiotics are not used; serious cases can be treated with antiviral drugs. Although less severe, the disease can present complications in people who have:
- HIV/AIDS
- Cancer
- Diabetes
- Pregnancy
- Chronic obstructive pulmonary disease (COPD)
Mycoplasma pneumonia – Other forms of pneumonia, including mycoplasma pneumonia, can be treated with antibiotics to kill the germs that cause the infection.
It is extremely important to rest during the treatment. In addition, it is not advisable to eliminate the cough; it helps to expel secretions that clog the airways. Therefore, do not take any cough medication without the advice of your doctor; cough syrups are generally not recommended. For cough and sore throat, it is better to drink a lot of water and natural juice.
Pneumonia Alternative treatment
Garlic – Chop and soak two cloves of garlic in ½ cup of distilled water in the evening; drink the solution tomorrow morning on an empty stomach. This remedy is also excellent for all forms of arthritis. Do not add more garlic when you just start, it can make you vomit.
Sesame seeds – take an infusion of Sesame seeds by steeping 15 gm of seeds in 250 ml of water. Mix the infusion with 1 tsp of linseed, 1 tsp of honey, and a pinch of table salt.
Hot tea – Drink a hot tea made with ginger, cinnamon and garlic (good remedy).
Fruits and vegetable juice – drink plenty of the following homemade fresh juice: carrot, radish, watercress and lemon; for best result, use a power juicer (juice extractor).
Pneumonia Prevention
You can prevent all forms of pneumonia by living a healthy lifestyle and get vaccinated; pneumococcal vaccine is an effective preventive mean against bacterial pneumonia. Talk to your doctor about this vaccine if you smoke or over 50.
In addition, there are preventive measures that can help you avoid not only pneumonia but also many forms of contagious diseases:
- Do not smoke
- Sleep well
- Exercise regularly
- Well nursing your child
- Eat lots of fruits and vegetables
- Discard used tissues
- Wash your hands regularly
- Do not share anything with a person suffering from a contagious disease including pneumonia
- Avoid wet kissing with anyone suffering from a contagious disease
- Cover your mouth when you cough, and do not let anyone cough in your face
- Treat gastro-oesophageal reflux disease (GERD) at early stage.



