Table of Contents
Angina
Angina pectoris (commonly called angina) is a chest pain due to poor blood oxygen supply to the heart muscle (myocardium). The pain may irradiate to the neck, lower jaw, shoulders, arms or back.
 In the developed countries, angina represents a major health concern; it is a sign of an underlying heart problem. You cannot feel angina symptoms without suffering from Coronary artery disease (CAD), or other heart related problems. That is why scientists always say angina is not a disease but a symptom of heart disease.
In the developed countries, angina represents a major health concern; it is a sign of an underlying heart problem. You cannot feel angina symptoms without suffering from Coronary artery disease (CAD), or other heart related problems. That is why scientists always say angina is not a disease but a symptom of heart disease.
There are different types of angina: stable angina, unstable angina and variant angina or Prinzmetal angina.
Stable angina – it is the most stable and most common type of angina. As its name says it, “Stable”, stable angina has a regular pattern, which makes it easier to be predicted. Stable angina is characterized by less frequent pain triggered by certain physical activities. Usually, the pain goes easily away by taking medicines.
Unstable angina –unlike Stable angina, the symptoms are unexpected, and may occur while at rest. The pain is more severe and difficult to go away even when taking medicines. Unstable angina indicates a high risk of myocardial infarction (heart attack); it requires immediate medical attention. If left untreated, unstable angina can result in cardiac arrest leading to sudden death.
Variant angina pectoris or Prinzmetal angina – Attacks are painful and occurs only at rest, usually at dawn.
Angina Causes and Risk Factors
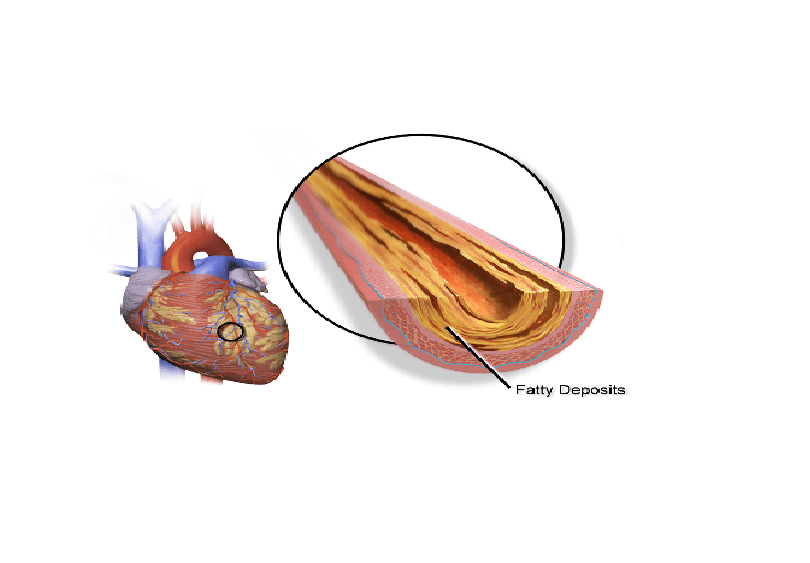
Angina is due to an abnormal narrowing of one or many coronary arteries (vessels that bring oxygenated blood to the heart muscle). In most cases of stable angina and unstable angina, the Blockages occur during efforts, when the heart needs more oxygen to provide energy for its work. Narrowing or blockage of the coronary arteries is usually due to atheroma (degenerative accumulation of fat in the inner artery walls), which main factors are:
- Age
- Sex
- Hypertension
- Diabetes
- Obesity
- High cholesterol
- Smoking
- Heredity.
Variant angina is linked to a spasmodic contraction of a normal coronary artery. The spam provokes a spontaneous blockage, which prevent blood from flowing to the heart. Unlike stable and unstable angina, Variant angina may occur in people with or without coronary artery disease (CAD).
The following are some other causes of spasms in the coronary arteries: emotional stress, cigarette smoke, drugs that narrow blood vessels (certain antimigraine drugs), over use of cocaine, etc.
Angina Symptoms and Warning Signs
Angina occurs during an effort by a feeling of discomfort behind the breastbone, which may irradiate to the neck, lower jaw, shoulders, arms or back. Complications of angina lie in myocardial infarction. The infarction results in an attack painful, intense and prolonged, accompanied with sweating, nausea or vomiting and malaise (hypotension); it requires immediate transport by ambulance to a specialized Emergency Cardiology Services.
Angina Diagnosis
The diagnosis is mainly clinical; it is based on the characteristics and duration of the pain and other risks of atheroma (fatty deposit in artery walls). The cardiologist may also search for changes in the electrocardiogram during the pain (Echocardiography). Other tests that can be done to search for lesions in the coronary arteries include: myocardial scintigraphy, enable to see if the heart is being fully vascularized by the coronary arteries; coronarography, a medical imaging technique used in cardiology to see the coronary arteries; and stress test on bicycle or treadmill, which may trigger painful symptoms.
Angina Treatment
 Stable angina is treatable with drugs: isosorbide dinitrate, nitroglycerin, aspirin, etc. unstable angina can be life threatening; it requires hospitalization for reducing the risk of a heart attack. Two other therapeutic methods are possible; the cardiologist can choose either
Stable angina is treatable with drugs: isosorbide dinitrate, nitroglycerin, aspirin, etc. unstable angina can be life threatening; it requires hospitalization for reducing the risk of a heart attack. Two other therapeutic methods are possible; the cardiologist can choose either
Coronary angioplasty – a medical procedure performed by a surgeon specialist to restore blood flow to the heart when the coronary arteries have become narrowed or blocked;
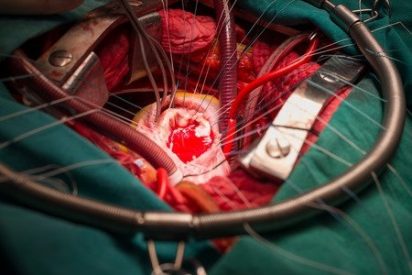
Aortocoronary Bypass (bypass surgery) – a surgical procedure consists of grafting veins and other canals shunting blood from the aorta to branches of the coronary arteries.
The choice depends on the results of the coronarography and the medicines. Variant angina requires a specific treatment. Vasodilators of the family of calcium channel blockers are shown to be effective in most cases.
Angina Prevention
The best Angina prevention is to avoid any form of degeneration of the walls of the arteries by living a healthy lifestyle: regular exercise, eating a diet, stopping smoking, and others.
References
1.COURAGE Trial Research Group (2007). “Optimal Medical Therapy with or without PCI for Stable Coronary Disease”. N Engl J Med 356: 1503–1516. doi:10.1056/NEJMoa070829. PMID 17387127. Retrieved 1 December 2014.
2.Tobin, Kenneth J. (2010). “Stable Angina Pectoris: What Does the Current Clinical Evidence Tell Us?”. The Journal of the American Osteopathic Association 110 (7): 364–70. PMID 20693568.
“MerckMedicus : Dorland’s Medical Dictionary”. Retrieved 2009-01-09.
Podrid, Philip J (November 28, 2012). “Pathophysiology and clinical presentation of ischemic chest pain”. UpToDate. Wolters Kluwer.(registration required)
The Crucial Role of Iron in the Body
6. Vaccarino, V. (16 February 2010). “Ischemic Heart Disease in Women: Many Questions, Few Facts”. Circulation: Cardiovascular Quality and Outcomes 3 (2): 111–115. doi:10.1161/CIRCOUTCOMES.109.925313. PMC 3012351. PMID 20160161