Table of Contents
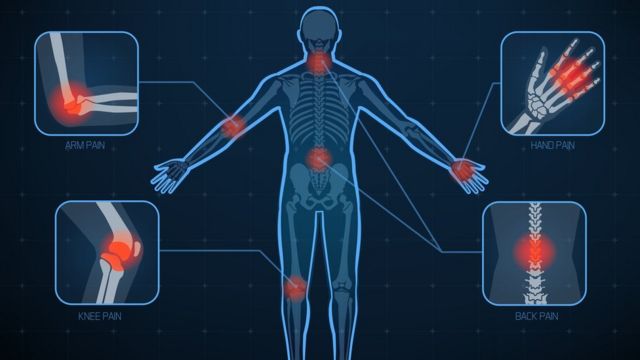
Rheumatic Fever is an inflammatory disease resulting from infection with streptococcus, a bacterium responsible for numerous pyogenic infections. The disease is characterized by inflammation of the heart and large joints: hands, wrists, knees, feet and sometimes the articulations of the elbows, hip, ankle and the top of the spine. In rare circumstances, rheumatic fever can possibly cause damage to other organs such as skin, lungs, eyes, and blood vessels.
Rheumatic fever occurs mainly in children 4 to 15 years. It is often caused by complications or an untreated group A streptococcal infection. Although the rheumatoid arthritis symptoms can be controlled, it can cause severe pain and joint deformities that hamper your professional and daily activities or your child school activities.
According to WHO, rheumatic fever and its cardiac complication, rheumatic heart disease, are annually responsible for nearly 400 000 deaths, mainly among children and young adults. It is estimated that the disease currently affects at least 12 million people around the world, including 2 million who require repeated hospital admissions and 1 million for which a cardiac surgery.
Rheumatic Fever Symptoms
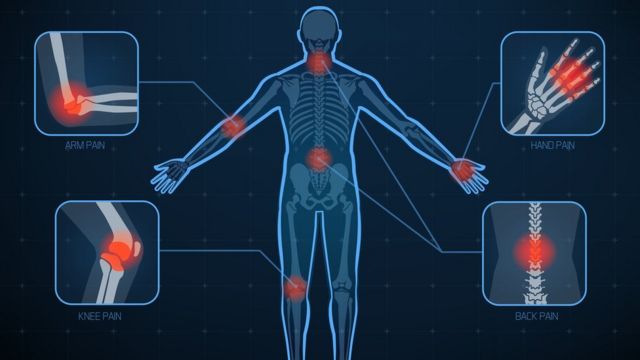 Typically, rheumatoid fever occurs 2 to 3 weeks after the onset of an untreated or poorly treated strep throat. It is a symptomized by rheumatoid arthritis (a form of arthritis which affects five or more joints) and high fever. In general, early in the disease, the large joints (ankles, knees, elbows or wrists; rarely feet, hips and hands) are affected; they increase volume and become hot, red, swollen, painful, and sometimes mobile.
Typically, rheumatoid fever occurs 2 to 3 weeks after the onset of an untreated or poorly treated strep throat. It is a symptomized by rheumatoid arthritis (a form of arthritis which affects five or more joints) and high fever. In general, early in the disease, the large joints (ankles, knees, elbows or wrists; rarely feet, hips and hands) are affected; they increase volume and become hot, red, swollen, painful, and sometimes mobile.
Heart problems are also common. If you have rheumatic fever, you have nearly 75% risk, in the first week, of developing rheumatic carditis, an Inflammation of the heart, mainly the pericardium, myocardium or endocardium. This inflammation can lead to formation of scar tissue, a medical condition that is often responsible for long-term valvular insufficiency, mitral regurgitation or rarely aortic aneurysm.
You can experience skin problems such as maculopapular rash (reddish spots for instance) or Meynet’s node (subcutaneous nodules appear in the area of the joints). As the disease worsens, you may also experience symptoms of:
- Fatigue
- chest pain
- rapid heartbeats
- shortness of breath
- painless rash associated with erythema marginatum
- uncontrollable body movements in the hands, feet and face, arms or legs.
Complications
Poorly treated or if left untreated, rheumatic fever can develop to serious complications, which can include hemodynamic instability commonly associated with an abnormal blood pressure and heart failure. Although are, there may be migration of germs in the valves of the heart leading to endocarditis, inflammation of the internal envelope of the heart, the endocardium.
Rheumatic Fever Causes
Rheumatic fever is the result of a combination of a streptococcal infection and Immunodeficiency (immune deficiency). Typically, rheumatic fever develops after a week of a strep throat or respiratory tract infections caused by Group A Streptococcus bacteria.
Group A strep bacteria tend to spread in the blood and accumulate in the joints, central nervous system (brain and spinal cord) or the heart. Their favorite location in the heart is often the valves that regulate the blood flow in the cavities of the heart. Once installed, the bacteria cause an infection of the inner part of the heart called endocarditis. There are two factors seem involved in the development of rheumatic fever:
Age – rheumatic fever occur mainly among children between 4 to 15 years old.
Immune deficiency – the immune system is the natural defense of your body; it protects against harmful organisms (viruses, fungus, bacteria, etc.) and all pathogenic substances. Once the Streptococcus bacteria are indicated in your body, the immune system reacts by attacking them. In some cases, unfortunately, the cells that normally destroy the bacteria also destroy the normal tissue of the joints on which the bacteria accumulate; this causes an inflammation of the joints and heart. If left untreated or poorly treated, eventually this condition will seriously damage the valves, increasing the risk of subsequent cardiac problems and the nervous system disorders.
Diagnosis
The diagnosis of rheumatic fever is based on clinical signs, biological exams (blood test) and imaging techniques.
Physical exam – the physical exam is the first step in rheumatic fever diagnosis. Your physician will examine your body to look for signs indicating the disease:
- Skin nodules
- Swollen joints
- Shortness of breath
- Abnormal heart function.
Blood test – the goal of the blood test is to detect in the blood evidence of certain proteins: Anti-streptolysin O (ASO or ASLO), antistreptokinase and antistreptodornase; these substances often produced in response to an infection by the streptococcus. The inflammatory process is confirmed by a Sed rate or erythrocyte sedimentation rate (ESR), a blood test used to examine inflammatory activity in the body.
Echocardiography – this is an imaging technique used to create a moving picture of the heart. This exam is important in the detection of inflammation or other disorders in the heart. It helps to reveal presence of many heart problems, including problems related rheumatic fever.
Electrocardiogram – also known as ECG, an electrocardiogram is a radiographic method performed to graphically represent the electrical activity in the heart. This test is often used in the diagnosis of rheumatic fever; it is quick (takes several minutes), painless and non-invasive. In addition, it is devoid of any side effects.
Rheumatic Fever Treatment
There is not miracle cure for rheumatism; treatments aim at relieving the pain, reducing inflammation, slowing the onset of joint damage, preserving function and mobility of the joints and taking non-medical measures that can improve the quality of your life. It is important to ensure that drug treatments are associated with bed rest.
Bed rest – a few weeks of rest is essential during rheumatic fever treatment. If you have complications such as heart problems, your rheumatologist may recommend you to stay in bed for about 3 months.
Antibiotics – antibiotherapy is an important and effective method that your physician can use to treat rheumatic fever; penicillin is one of the best antibiotic against streptococcus. It is given, intravenously, in high doses in the first 10 days; usually, your doctor will consider 1 to 2 million units IV per day. Treatment should be continued as recommended by your doctor to prevent recurrences.
Anti-inflammatory – your rheumatologist may prescribe corticosteroid at dose of 2 to 2.5 mg/kg/24 hours for 4 weeks: if the clinical examination and sedimentation rate become normal for at least a week, the dosage may be slowly reduced but not stopped. To reduce the risk of recurrence, your doctor will give you a treatment of aspirin (5cg/kg/day) started two weeks before and continued two weeks after stopping the anti-inflammatory treatment.
Anticonvulsants – if you have uncontrollable body movements in the hands, feet, face, arms or legs, it is most likely that you will be recommended to take anticonvulsants medications:
- Valproic acid (Depakene, Stavzor)
- Carbamazepine ( Equetro, Carbatrol).
Side effects of those drugs may include but not limited to vomiting, loss of appetite, fever, dark urine, drowsiness, dizziness, liver disorders (hepatitis for instance), or low red and white blood cell counts.
Rheumatic Fever Prevention
If you have strep throat, see your health care provider and follow the treatment as prescribed. Rheumatic fever is often the consequence of untreated or poorly treated strep throat. Prevention of recurrences is based on oral or Intramuscular injection of antibiotics for at least 5 months.